At WiseGEEK, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What Should I Expect from a Neurological Examination?
A physician performs a neurological examination to test how well a patient’s nervous system is functioning. The nervous system is a network of nervous tissues which must accept and process sensory input, and then produce a response to the stimuli. Sensory input includes factors both external and internal to the body, including pain, temperature, taste, pressure, blood pH, light, hormone levels, and sound, amongst other stimuli. If a patient or physician suspects the nervous system may be impaired, a doctor may perform a neurological examination to screen for possible problems. The exam consists of several parts; an assessment of general appearance, mental status, cranial nerves, motor system, sensory system, reflexes, and finally, coordination and gait.
A doctor will likely begin a neurological examination by talking to the patient and noting the patient’s posture, alertness, and motor skills. Motor skills are the body’s ability to move efficiently. A doctor will be particularly on the lookout for tremors called fasciculations, sudden, jerky movements called chorea, and sustained contractions of the mouth, eyes, tongue, back, or mouth called dystonia. Vital signs, such as blood pressure and heart rate, obesity, abnormal thinness, deformities, and abnormal proportions, such as wide-set eyes or low-set ears, should also be noted.

The mental status portion of a neurological examination consists of several questions that test a patient’s ability to think properly. This may include exercises in drawing, writing, reading, obeying commands, and memory. Any changes in intellectual capacity or speech patterns, such as the ability to speak fluidly, should be evaluated, as they may be signs of a neurological problem.

The physician then puts the patient through several tests that help evaluate the individual function of the cranial nerves, which supply motion and sensation to the face. Eye motion, pupil dilation, vision in each eye, smell through each nostril, facial muscle function, tongue function, swallowing, and sensation in different parts of the face are examined with special attention on symmetry. Movement, appearance, and sensation should be equal on both sides of the face.

The motor system phase of the neurological examination assesses muscle strength and tone throughout the body. The patient will likely undress for this exam, as the physician needs to evaluate the appearance of muscles, looking for over-development or muscle atrophy. The physician may ask the patient to flex and extend muscles, fan out the fingers, grasp objects, and use muscles against resistance.

The sensory exam tests the patient’s ability to feel pain, temperature, position, and light touch. Tests may include a pinprick, asking the patient to close his eyes and identify a number written on his back or palm, or close his eyes and identify where on his body he is being touched. A problem with the sensory system may point to such disorders as thiamine deficiency, neurotoxin damage, or diabetes mellitus.

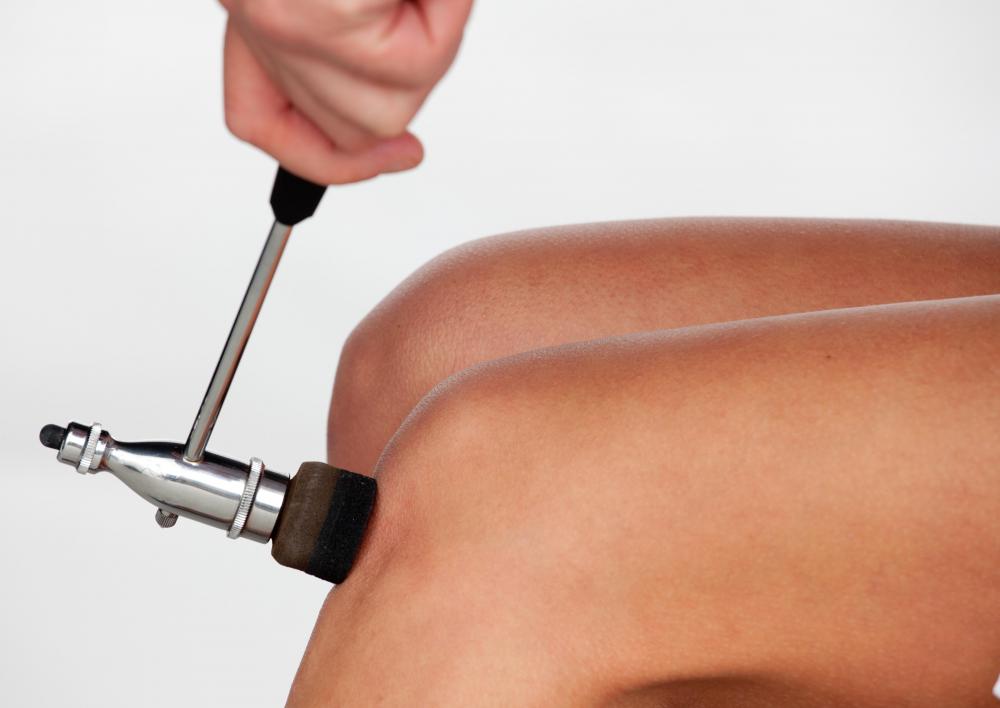
The physician will then test the patient’s reflexes, the body’s involuntary responses to stimuli. Usually this is done with a small reflex hammer that is hit against tendons or muscles in the body. The classic example of this test occurs when the tendon just below the knee is hit, causing a kick of the lower leg.
The final tests in a neurological examination include coordination, gait, and balance. To test coordination, a physician may ask the patient to repeat quick movements on command, touch a finger to his nose and then to touch a finger to the doctor’s fingertip, and slide the heel of the foot down the opposite shin. The doctor tests gait by evaluating the patient’s ability to walk smoothly, commanding the patient to walk normally, walk with one foot directly in front of the other, walk on the heels, and walk on the toes. Finally, the physician may perform the Romberg test, which asks the patient to balance while closing his eyes. If the patient cannot balance, it may be a sign of a neurological disorder.
AS FEATURED ON:
AS FEATURED ON:

















Discuss this Article
Post your comments