At WiseGEEK, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What is Prostate-Specific Antigen?
Prostate-specific antigen (PSA) is a protein that is produced by healthy prostate cells in men. The protein produced in the prostate and is secreted in the semen during ejaculation. A blood or urine test measuring levels of prostate-specific antigen is used by doctors as a means of examining a man’s prostate health, in conjunction with other methods of evaluation. The protein was first characterized in the 1970s, and the PSA blood test was developed in the 1980s. The first commercial PSA blood test was released in 1986.
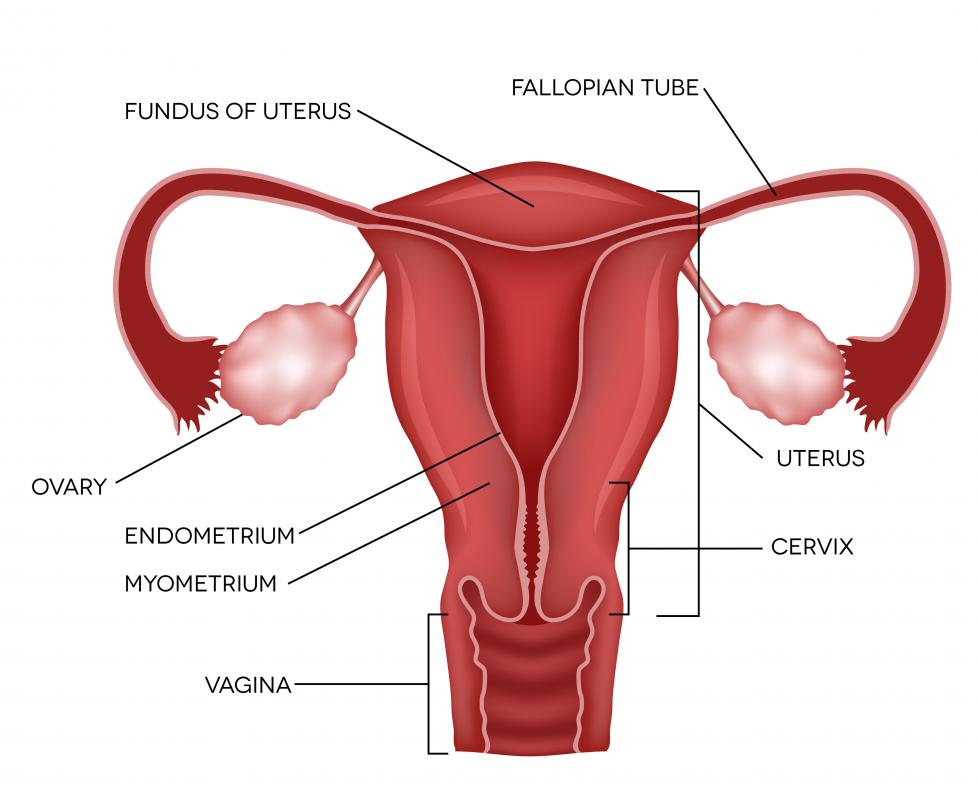
Prostate-specific antigen is a type of protein called a glycoprotein, which means that it contains a type of sugar chain called a glycan. This protein is produced by the prostate gland for inclusion in semen, the white fluid ejected from the penis during ejaculation. PSA, which is also known as seminin and seminoprotein, improves sperm motility by liquefying semen. In addition, the protein helps to dissolve the cap of mucus that is present in the cervix, which allows sperm to enter the uterus.

Since the discovery and characterization of the protein in the 1960s and 1970s, it has been made clear that the common name for the protein, prostate-specific antigen, is actually inaccurate. This is because the protein can be found in other tissues of the body, and even in women. In addition to the prostate gland and semen, PSA has also been found in female ejaculate, amniotic fluid, breast milk, breast tissue and the salivary glands. Despite this, the PSA test is still valid for the purposes of evaluating prostate health because levels of the protein are elevated in men who have prostate cancer and other prostate-related conditions.

There is some controversy regarding the use of the prostate-specific antigen test for evaluating prostate health. One reason is because elevated levels of PSA are not caused only by prostate cancer. Only about one-third of men who have a positive PSA test actually have prostate cancer. The prostate naturally enlarges with age, and other urogenital diseases can also cause prostate enlargement, so other tests such as physical examination and ultrasound are used in addition to the PSA blood test to make an accurate diagnosis.

Another aspect of the controversy is that some studies indicate that the PSA screening test is not useful for reducing mortality because of prostate cancer, and that the long-term benefits for patients are uncertain. These studies have concluded that extensive PSA screening results in unnecessary treatment for non-existent prostate problems, leading to chronic problems such as infection, erectile dysfunction and urinary incontinence. Many public and private medical organizations acknowledge these issues and suggest that men talk with their doctors about PSA screening to weigh the risks and benefits.
AS FEATURED ON:
AS FEATURED ON:















Discuss this Article
Post your comments