At WiseGEEK, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What is Hospital-Acquired Pneumonia?
Hospital-acquired pneumonia (HAP) is a lung infection that may be contracted within 48 hours following hospitalization. Often caused by exposure to pathogens within the hospital setting, such as gram-negative bacilli and staph infection, HAP is considered a more serious form of traditional pneumonia. Treatment for this potentially life-threatening condition includes the use of antibiotics to treat infection and, in some cases, supplemental oxygen to aid breathing.
There are three subdivisions of illness associated with hospital-acquired pneumonia: postoperative pneumonia, ventilator-associated pneumonia (VAP), and health care-associated pneumonia (HCAP). A commonality among all forms of HAP is that an individual acquires infection while he or she is in a health care facility, such as a hospital or clinic. Individuals with HAP generally exhibit the same symptoms as she or he would had his or her exposure to pathogen-induced pneumonia occurred out in the community. The only difference between HAP and traditional pneumonia is the severity of symptom manifestation.

Individuals who have been hospitalized may already be experiencing compromised immunity, which makes them more susceptible to gram-negative bacilli and staph infection. An increased susceptibility may oftentimes be accentuated by additional risk factors. Individuals who suffer from alcoholism, chronic illness, or advanced age are at an increased risk for developing HAP following hospitalization. Additional elements that may put an individual at risk may include recent surgery and the use of medications that suppress the immune system.

Those who develop hospital-acquired pneumonia may experience a range of symptoms that may manifest to varying degrees. Common signs of pneumonia such as fever, fatigue, and chills are often the first to occur. Individuals with HAP may also develop nausea, joint discomfort, and breathing difficulty. Other signs indicative of HAP may include loss of appetite, a greenish tinge to mucus and phlegm, and chest pain that occurs when coughing or breathing deeply.

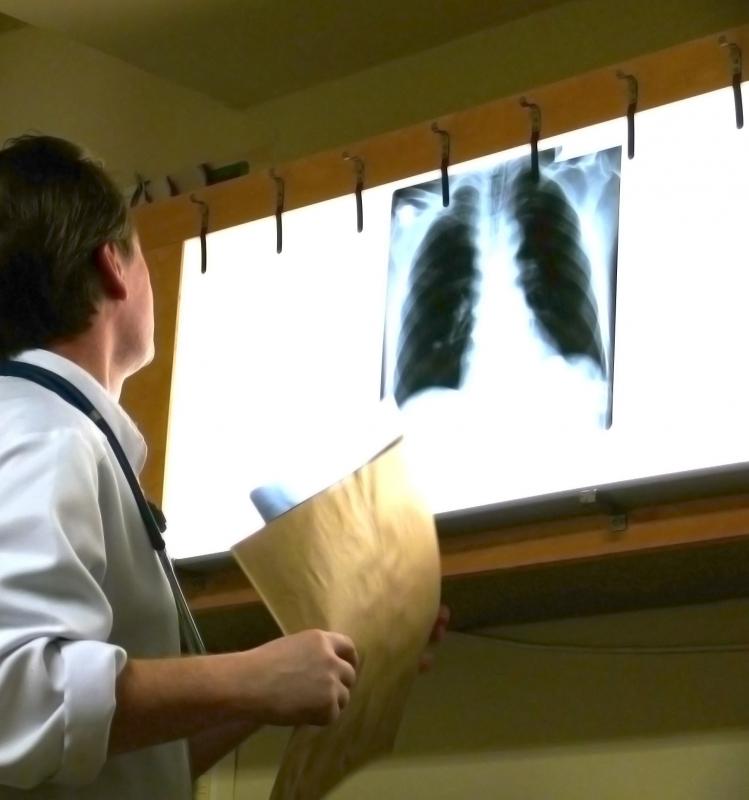
There are several tests that may be employed to confirm a diagnosis of hospital-acquired pneumonia. In addition to a physical examination that may indicate respiratory issues, such as fluid buildup in the lungs, an individual may undergo blood and imaging testing. A complete blood count (CBC) may be performed to evaluate red and white blood cell count and hemoglobin levels. Samples of sputum may be obtained from the bronchi and lungs of those whose mucus is discolored to check for the presence of bacteria. Image testing that includes a computerized tomography (CT) scan and chest X-ray may be conducted to evaluate the condition of the individual's lungs.

Treatment for hospital-acquired pneumonia is centered on the administration of antibiotics to treat the infection. The kind of antibiotic used is dependent on the type of bacteria causing the infection, which is identified during analysis of the sputum culture. In some cases, supplemental oxygen may need to be administered to assist breathing. Additional treatments may be given to help break up mucus accumulation in the lungs and make breathing easier.

Individuals of advanced age or those who do not respond well to treatment are at a higher risk for developing further complications, such as acute respiratory failure. Mortality rates associated with HAP are relatively high for those who acquire the condition through exposure to the pathogen gram-negative bacilli. With appropriate treatment, the prognosis associated with HAP is good and individuals often make a full recovery within two weeks.
AS FEATURED ON:
AS FEATURED ON:














Discussion Comments
I don't suppose a patient could later sue a hospital for giving him or her hospital-acquired pneumonia. It's not like the hospital can do any more about staph bacteria than a school or restaurant or other public building. When I was in the hospital for minor surgery, my nurse told me that some people are prone to ventilator associated pneumonia, and the nurses can't just stop the ventilator treatments because of it.
There was also a condition called aspiration pneumonia, often caused by patients inhaling their own vomit into their lungs. It was considered a chemical kind of pneumonia, not the same as the kind triggered by pneumonia bacteria. Let's just face it, if you have to spend time in a hospital, you're going to have to accept the fact that all of those risks are going to be present. No hospital can completely eliminate every single toxic substance in the building.
The first time I was ever admitted to a hospital, the doctor told me I would only be there for two or three days at the most. I asked him why and he said if I stayed any longer, I might actually get sicker. He told me about hospital-acquired pneumonia, and I was supposed to tell him right away if I started having breathing problems or developed a bad cough. Fortunately, I passed the kidney stone a day later and went home without any problems.
I did see some other people on the same floor who had to have breathing treatments every morning, including my elderly roommate at the time.
Post your comments