At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What Is Brain Calcification?
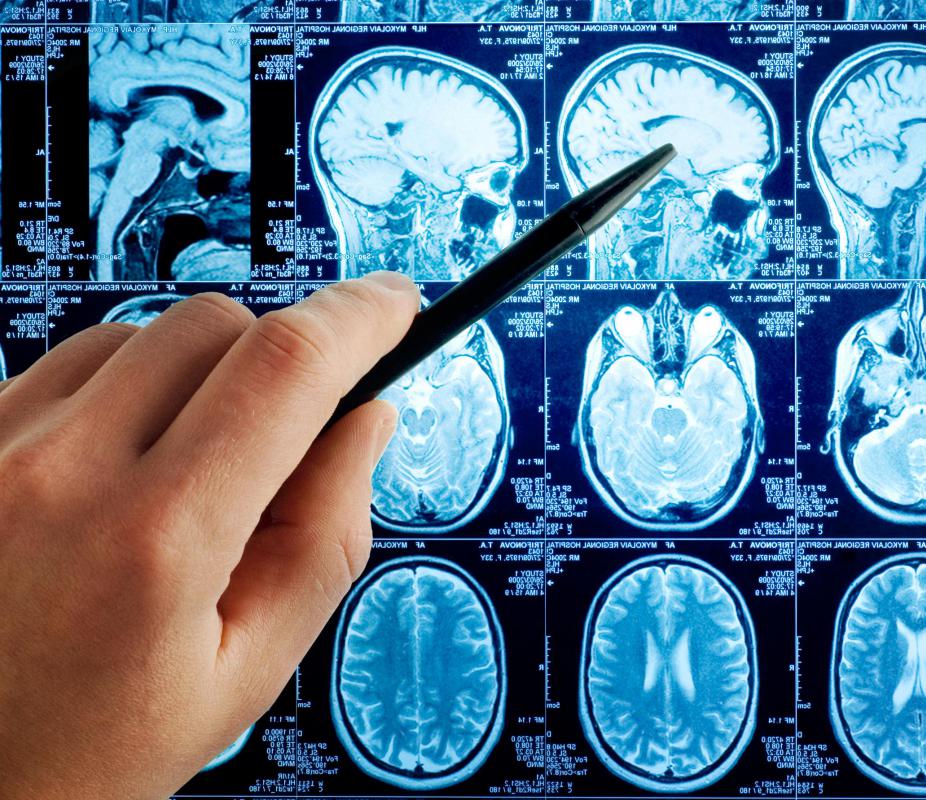
Nearly all of the calcium that enters the body typically is used to strengthen teeth and bones or is absorbed by the blood. When the balance between calcium and other chemicals in the body is off, calcium may be deposited elsewhere in the body. In the medical condition known as brain calcification, calcium is not absorbed as it usually is, but rather is deposited in the brain. Diagnosis of this condition may be made with a variety of procedures including x-rays, computed axial tomography (CT or CAT scan), or magnetic resonance imaging (MRI).
Brain calcification may be triggered by a variety of medical problems. It may be associated with stroke or brain injury, or it may occur in tumors in the brain. Hypoparathyroidism, in which levels of parathyroid hormone in the body are abnormally low, may also be associated with calcification.

Symptoms of brain calcification may or may not occur in any given person who experiences it. They depend on the amount of calcification as well as where the calcium is deposited in the brain. Fahr’s Syndrome, an inherited condition, is one common manifestation of calcification in the brain in which calcium is deposited in the cerebral cortex and the basal ganglia. The cerebral cortex plays a role in consciousness, memory, awareness, and other functions while the basal ganglia assists in motor control and eye movement among other functions.

Consequently, symptoms of brain calcification may include problems with any of these functions. Neuropsychiatric symptoms range from mild, such as faulty memory or degraded ability to concentrate, to more extreme, such as dementia or psychosis. These types of symptoms are often the first to be detected before diagnosis. Headache, vertigo, seizures, and problems with motion and coordination are also common.

While age does not reliably predict the amount of brain calcification or its impact on neurological function, Fahr’s Syndrome is usually diagnosed in patients in their 40s and 50s. There is neither a cure for Fahr’s Syndrome, nor a standard treatment protocol due to the wide range of possible symptoms. Predictions for the likely outcome of the disease are difficult to make and vary widely from patient to patient.

A course of treatment for a patient is generally developed based on his or her specific symptoms. Drug therapy may be prescribed for symptoms such as anxiety, depression, obsessive-compulsive behavior, and mental disorders. Anti-epileptic drugs may be prescribed to control occurrence of seizures. Patients are generally scheduled at least annually for ongoing assessment of their symptoms and review of and updates to their treatment plans.
Is Calcification on the Brain Serious?

Calcification on the brain can be an extremely serious medical condition and can have grave consequences for individuals who have it. Yet there is much to be determined when it comes not only to how and when calcium deposits in various parts of the brain occur but also what effects the calcification actually has.
Primary Familial Brain Calcification (PFBC) is a rare neurological disorder in which calcium deposits build up in the brain, often in the basal ganglia, which controls movement in the body. Studies have shown that PFBC may materialize in less than 10 in 1000 people. Of that small percentage, symptoms may never actually occur.
While some patients can be asymptomatic, others can suffer from everything from vertigo to migraines to dementia. The major red flags associated with PFBC are psychiatric issues and movement disorders. Research suggests that abnormally high levels of calcium in brain cells may change the brain chemistry in such a way as to lead to Parkinson's disease.
According to the Mayo Clinic, Parkinson's disease is caused by irregular brain activity that affects the production of dopamine. However, the precise nature of the cause of that irregular activity is still rather hazy. A study conducted by a team from the University of Cambridge posits that when the relationship between calcium and alpha-synuclein in brain cells changes, the affected person could develop Parkinson's disease.
Brain calcification can only be detected through imaging tests, the most common being a computerized tomography (CT) scan. Further, it really isn't looked for until symptoms arise. Movement-related symptoms can include tremors, involuntary tightening of the muscles, unsteady walking and slowness of movement. Psychiatric-related symptoms may include migraines, memory loss, personality changes, seizures, impaired speech, trouble concentrating, dementia or psychosis.
The short answer is that, yes, brain calcification can be tremendously distressing, in part because it is still a mysterious phenomenon and in part because symptoms often take decades to manifest themselves, at which point the calcified areas, which cannot be destroyed, have already created detrimental changes in the brain and the body.
Can Brain Calcification Go Away?
Though it can create neurological maladies that can be treated, there is no proven treatment for brain calcification. Once the calcification exists, it does not go away. Instead, it disrupts things and changes the way the brain functions. When this happens, doctors treat the symptoms to the best of their abilities, sometimes without a precise understanding of their origins.
The best chance that exists for the potential to diminish brain calcification is through collaboration among medical professionals. Take the case of an American woman who went to her primary care physician, complaining of trouble with lower extremity movement and word-finding difficulties. Her doctor ordered an MRI, which showed deep white matter calcifications. When the neurologists had trouble interpreting the data because they didn't quite understand what they were seeing, they consulted with a radiologist, who had seen such images before. Only then did the diagnosis and means of treatment reflect Fahr's disease, which is distinguished by irregular deposits of calcium in the brain.
This case shows how obscured calcification in the brain actually is. It is not yet fully understood, and until it is, the means by which to reduce it will remain elusive. Doctors do not yet know how to make it go away, so instead, they try to manage the symptoms, hoping to improve their patient's quality of life.
Is Brain Calcification Painful?
Pain is a slippery term when it comes to the potential effects of brain calcification, particularly because of the time over which symptoms manifest themselves and because of how people interpret pain. Perhaps it becomes a question of physical vs. psychic pain. Brain calcification can cause painful migraines, but it can also cause involuntary muscle movements. There are links between brain calcification and dystonia, which can range from mild to severe. Of course, dementia and Parkinson's Disease can cause many different types of pain. In addition to physical pain, people with brain calcification may experience emotional distress from the associated memory loss or loss of concentration. They may also undergo involuntary personality changes that could lead to severe mental anguish.
Another aspect of the psychic pain caused by brain calcification is having the knowledge and worry that something is wrong but not truly understanding the cause of the symptoms. Rather, it seems to be more like a game of whack-a-mole, in which symptoms are treated as best they can be when they pop up.
AS FEATURED ON:
AS FEATURED ON:














Discussion Comments
Our granddaughter has 5 dime and nickle size calcified tumors in her brain. First 3 discovered at age 12. She is now 14. Since age 2 she has been classified as having a progressive spastic paraplegic neurological disorder. Now she has diabetes, kidney complications and had a heart ablation at age 7. No conclusive diagnosis has ever been made. She suffers from extreme fatigue, shot term memory loss, uses wheelchair and walking canes. Has Baclafin pump in abdomen, latest problems: suffered mild stroke, swelling on brain. Headaches, mood swings and depression.
My understanding is that brain calcifications are not malignant. The only danger is if the calcification grows and starts to take over a meaningful amount of the fixed amount of space within the skull.
I wonder how common this is, especially among the older generations.
Post your comments