At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What Is Vestibular Nystagmus?
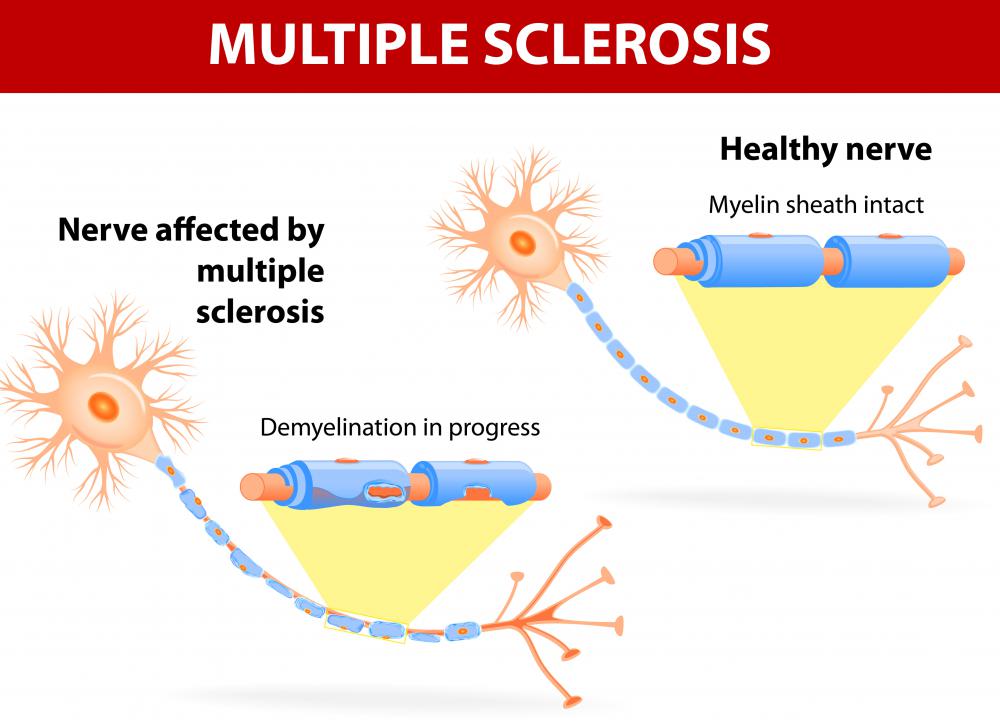
Individuals with vestibular nystagmus experience rapid involuntary eye movements triggered by a disruption of the signal pathways between the eyes, inner ear, and the brain. Vestibular nystagmus may be further broken down into the categories of peripheral or central, depending on the particular location of the problem causing the disorder. Eye movements might occur horizontally, vertically, or in a rotational pattern. Infections, lesions, and disease processes that include multiple sclerosis may cause the optical disorder. Medications used for treatment may resolve underlying conditions or provide general symptom alleviation.
The semicircular canals, deep within the ear, monitor the body’s physical position in space, sending signals to the brain when position changes occur. The brain responds by altering posture to ensure balance and stability. Nerves regulating vision also receive signals from the canals and transfer these to the brain when head position changes occur. Physicians refer to this function as the vestibulo ocular reflex (VOR). When abnormalities in the canals occur, the brain receives inappropriate signals that can affect eye movement and vision.

Peripheral vestibular nystagmus generally occurs because of malfunctions within the inner ear. The signal obstruction in one or both of the semicircular canals causes horizontal jerking movements of the eyes. If only one canal is afflicted, the eyes veer in that direction. Problems arising in both canals cause the eyes to wander back and forth horizontally. Depending on the severity of the abnormality, individuals may experience dizziness, nausea, and balance problems along with nystagmus.

Minute calcium carbonate crystals adhere to certain delicate membranes in the ear. Occasionally, these crystals detach because of normal aging, infections, or head trauma. The objects then wander into other areas of the inner ear when head movement occurs. Displaced crystals interfere with nerve tissue and disrupt the signals transmitted to the brain, causing nystagmus.

Central vestibular nystagmus happens as a result of abnormalities that occur on the receiving end of signal transmissions in the brain. Other types of nystagmus that are related to cranial abnormalities include down gaze, up beat, and seesaw nystagmus, which describe the direction of eye movement and may provide a clue to the location of the affliction. Symptoms of nystagmus originating from brain malfunction include rapid eye movements in horizontal, vertical, or circular motions. A number of disorders, including brain swelling, multiple sclerosis, and tumors, contribute to central vestibular nystagmus.

Ophthalmology specialists diagnose the disorder by tracking eye movement while a patient performs basic visual exercises. Physicians may perform electronystagmography, which records eye movement during testing. Reversing the underlying infection or irritation may correct vestibular nystagmus, and treating nystagmus may include taking a prescription antiemetic, anti-inflammatory, anticholinergic, or other medication, which slows signal transmission and brain response. Patients may also undergo a type of physical therapy that retrains the brain’s response to inappropriate signals.
AS FEATURED ON:
AS FEATURED ON:














Discuss this Article
Post your comments