At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What is Vaginal Dysplasia?
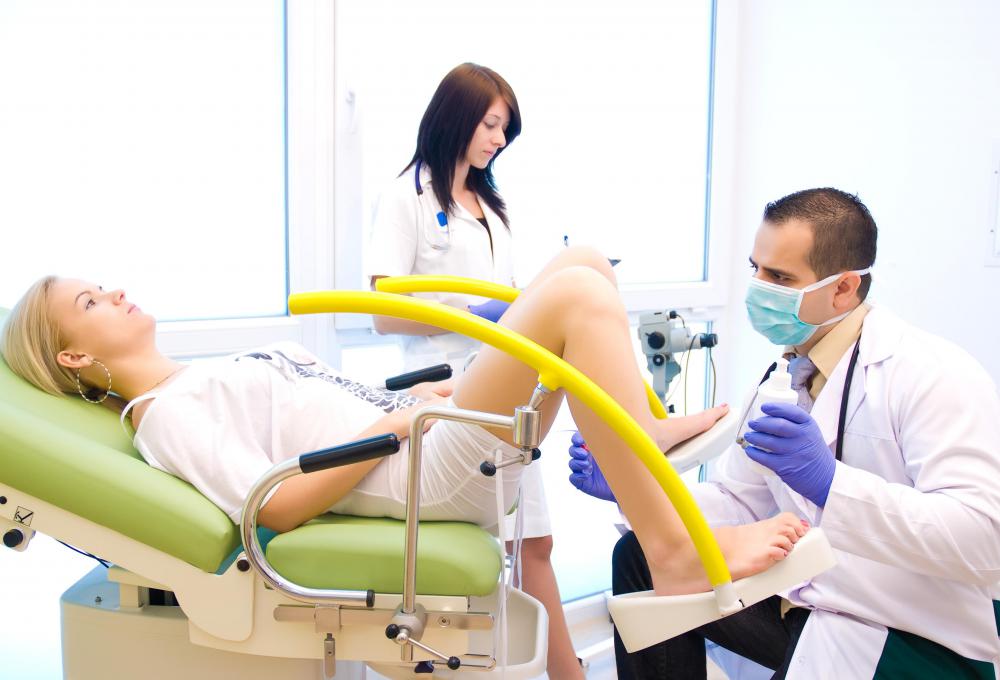
Vaginal dysplasia is the abnormal growth of cells within the tissue of the vagina. This is associated with human papillomavirus (HPV) infection and early stage development of vaginal cancer. It is generally detected during routine female exams, which include a pelvic exam and Pap smear. Women who experience discomfort or irregular menstruation may be symptomatic and should seek medical attention. Annual female examinations and responsible sexual practices decrease a woman's chances of developing this form of dysplasia.
Human papillomavirus is an infection that causes abnormal cell maturation and manifests as either genital warts or lesions. Though it can affect any part of the body, a genital HPV infection commonly occurs in women under the age of 25 who have a weakened immune system. Having multiple sexual partners is also a risk factor, even if a person always uses protection, as HPV can be spread through areas that are not covered by a condom. As HPV often does not cause symptoms, it can be difficult to know whether a person has it, even if he or she practices safe sex. Transmitted through direct sexual contact, vaginal dysplasia associated with HPV can result in the formation of pre-cancerous lesions.

Detected during a Pap smear, HPV-related dysplasia is classified as low- to high-grade, depending on stage of development. Abnormalities classified as low-grade generally subside over time. Serious grades, such as moderate and high, require treatment, which may include surgery to remove the affected cells and tissue. Other treatments may include cryotherapy, which involves the freezing of the affected tissue to eliminate abnormal cells, laser surgery, and electrocautery, which uses a high-frequency electrical current to remove affected cells. It's rare for dysplasia to develop into cancer; however, a woman who experiences repeated infections has an increased chance of developing vaginal or other gynecologic cancers.

Vaginal cancer is a rare condition resulting from the generation of abnormal cells that do not die as do normal cells during healthy cell production. The numerous cells accumulate in masses, forming tumors, and have the potential to metastasize, or separate and spread to other parts of the body. Women who have vaginal cancer may not exhibit any symptoms, so early detection is key.

As with HPV, pre-cancerous vaginal dysplasia is generally discovered during a routine pelvic exam and Pap smear. There are no specific tests designed exclusively to detect vaginal cancer. Women who experience unusual vaginal bleeding, painful urination, or pelvic pain may be exhibiting symptoms associated with the early stages of cancer and should undergo a physical exam. In addition to a routine female exam, other testing may include a biopsy of the vaginal tissue and a colonoscopy.

In the event that cancerous cells are discovered, additional diagnostic testing is required. A positron emission tomography (PET) scan is conducted to determine the extent of the cancer and whether or not it has metastasized. An additional biopsy and imaging tests are also conducted to determine the staging, or degree, of the cancer. Treatment for vaginal cancer is dependent on the type and staging associated with individual diagnosis. There are no typical guidelines for treatment, but options may include surgery to remove cancerous lesions or tumors, internal or external radiation therapies, and chemotherapy.

Women who have had HPV, smoke, or have had multiple sexual partners are at an increased risk of developing vaginal cancer. Those who have vaginal intraepithelial neoplasia (VAIN), have been exposed to the drug diethylstilbestrol (DES), or have been treated for other forms of gynecologic cancers are also at an increased risk. The prevention of HPV-related infection through responsible sexual practices, such as monogamy and using condoms, may decrease a woman's risk of developing vaginal dysplasia. The vaccination Gardasil® was approved by the Food and Drug Administration (FDA) in 2008 for the prevention of HPV and vaginal cancers related to infection.
AS FEATURED ON:
AS FEATURED ON:














Discussion Comments
To anon275849: Since there is no date on your post, this response may be long after the fact. I had uterine cancer and grade III vaginal dysplasia. A complete hysterectomy was done but only removal of the dysplasia, which is precancerous. Not knowing your full condition, the doctor's recommendations sound a bit extreme. I'd certainly get a second opinion.
I have been diagnosed with vaginal dysplasia and my gyno wants to do a complete hysterectomy and vaginal reconstruction. Has anyone gone through this?
I am confused as to why I have been diagnosed with vaginal dysplasia. None of the risk factors apply, having been married for 41 years and neither my husband nor I have had other sexual partners. I have never had HPV nor ever smoked. This is the first time that a pap test result has come back as abnormal. I have had a hysterectomy many years ago. Therefore, I have no uterus or cervix.
yes, i believe that to be very likely. very similar to my story.
about three years ago I stayed the home of an old friend who was receiving treatment for vagina dysplasia. A few weeks after I returned I had some symptoms in the vagina and I was treated for thrush. Some time later I developed a small wart. It started to grow a sample has been taken and it has cancerous cells. Is it possible this was passed using the same toilet facilities? I take immunosuppressants.
Post your comments