At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What Is the Treatment for Eosinophilia?
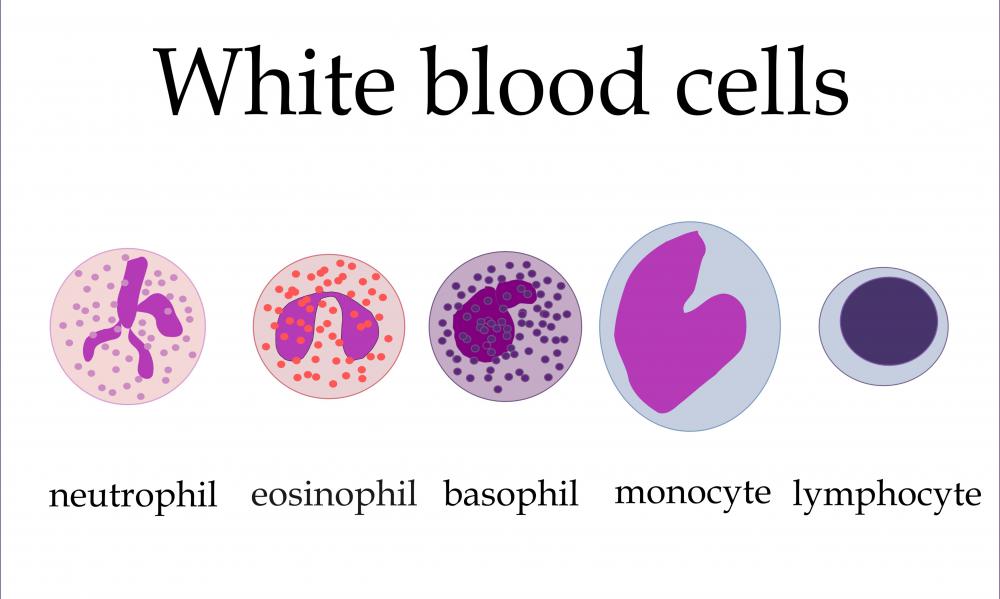
Treatment for eosinophilia depends on whether the condition is considered secondary, clonal, or idiopathic. The condition may produce symptoms anywhere in the body and occurs because of an abnormal number of granulated white blood cells known as eosinophils are present. Secondary and clonal eosinophilia generally reverses after the underlying contributing factors are treated. The idiopathic disease process usually requires medication that reduces inflammation and interferes with cell growth and development.
Eosinophils normally number 100 to 300 per deciliter (dl) of blood. When this count rises to 500 cells/dl or more, health care providers call the condition eosinophilia. Mild cases of the condition occur when eosinophils escalate to between 500 and 1,500/dl. Severe cases occur when these levels surpass 1,500/dl. If a patients has 1,500/dl of eosinophils for three months or longer, the condition becomes hypereosinophilia.

Secondary eosinophilia occurs when the granulated white blood cells respond to an allergic reaction, antimicrobial or parasitic infection, or injuries or a disease process that causes an inflammatory response. Treatment for eosinophilia in this instance generally requires resolving the underlying condition. Clonal eosinophilia is the body's response to benign or malignant growths and to hemolytic conditions that include leukemia. Removing benign growths usually decreases the eosinophil count. Often the chemotherapy and cytotoxic medications used to treat malignancies act as an effective treatment for eosinophilia.

Physicians diagnose idiopathic eosinophilia by ruling out any causative factors that may include abnormal growths, infections, or tissue inflammation. Causes of eosinophilia include familial traits and genetic mutations. As affected blood passes through the organs, eosinophils cause tissue damage in these regions. Left untreated, the disease may produce irreversible organ damage or progress into certain types of leukemia.

Managing eosinophilia generally includes the use of corticosteroids, which reduce inflammation, and the antineoplastic medication, hydroxycarbamide, which inhibits cell replication. Physicians might also use interferon-A, which also inhibits cell division. Some patients respond to the cytotoxic, tyrosine kinase inhibitor, known as imatinib, as part of treatment for eosinophilia. Organ damage may require reparative surgery or secondary medications to alleviate symptoms.

Symptoms vary from patient to patient, but visible signs of eosinophilia can include skin rashes that resemble eczema or hives. Elevated numbers of eosinophils in the heart can produce blood clots that break free and travel through the body, causing pulmonary embolism or stroke. Patients experience chest pain or tightening, cough, and swelling in the feet and legs. Cardiac tissue may become fibrous and valve damage occurs. The condition may progress to congestive heart failure.

When it affects the lungs, eosinophilia may produce symptoms similar to respiratory infections, and imaging studies may reveal infiltrated or inflamed tissue. Blood clots or fibrous tissue may develop, further impeding breathing ability and tissue oxygenation. Gastrointestinal symptoms of eosinophilia often include abdominal pain accompanied by nausea, vomiting, and diarrhea. Some patients also develop an enlarged liver and spleen. Central nervous system effects of the disease process include behavioral changes, a decline in cognitive abilities, confusion, and memory loss.
AS FEATURED ON:
AS FEATURED ON:
















Discuss this Article
Post your comments