At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What Is the Treatment for a Prolapsed Bowel?
The treatments for a prolapsed bowel can include a change in diet, taking stool softeners, and surgery. This condition can occur as a result of straining during bowel movements. Increased fiber and stool softeners can reduce the need for muscle strain, and allow the body to heal itself. In extreme situations where the body is unable to repair the damage internally, surgery may be required to reattach the lower portion of the large intestine, or strengthen the walls of the vaginal canal, so that the bowels are held in place without the risk of becoming unattached again.
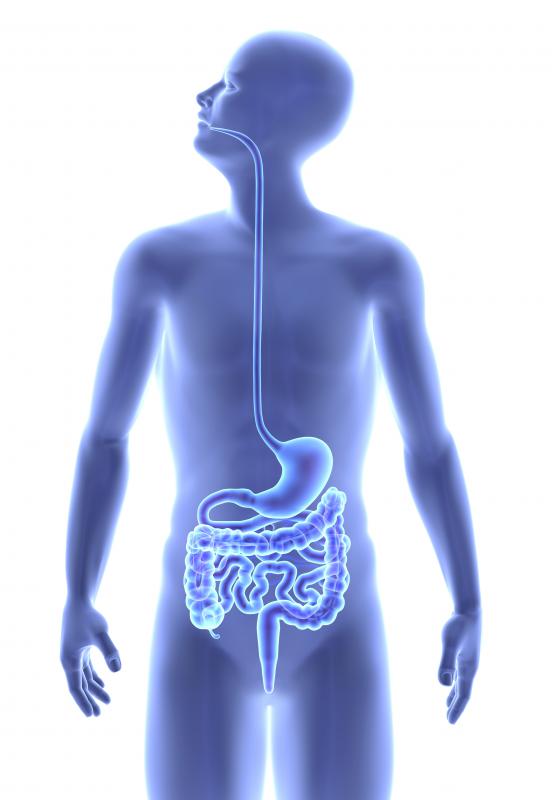
The term prolapsed bowel may be used to refer to three different types of pelvic tissue failure and can effect the large and small intestines. Rectocele and enterocele, two conditions which are unique to women, affect portions of the large and small intestine respectively and occurs when the tissue walls of the vagina begins to weaken. Portions of the intestines begin to press and sometimes protrude against the back and upper walls of the vaginal canal as a result. Rectal prolapse, which can affect both men and women, refers to the lowest portion of the large intestine becoming dislodged and sometimes protruding from the anus. Weakened pelvis muscles can be a side effect of giving birth, undergoing abdominal surgery, or aging.

The most common form of treatment for a prolapsed bowel involving rectocele and enterocele is surgery during which the weakened tissues of the vaginal canal are strengthened and repaired. This surgical procedure is usually performed through the vagina under general anesthesia, and no abdominal incisions are necessary. Patients may be required to remain in the hospital for two days to monitor for signs of infection. Recovery time may last six weeks before normal activities and sexual intercourse are resumed. Normal bowel functions resume between two and four weeks following surgery.

Treatment for prolapsed bowel involving the rectal muscles may include an adjustment to a patient's bathroom habits in addition to surgery. Straining during bowel movements and hemorrhoids can contribute to and cause rectal prolapse. A patient's doctor may begin by increasing the amount of fiber present in the patient's diet, encouraging her to drink more water, and prescribing stool softeners that reduce the need for strain. Topical creams and prescription medications are also available to reduce the effects of hemorrhoids, which tend to put pressure against the rectum. In some cases the hemorrhoids may need to be removed surgically and the rectum reattached.

Surgical repair for a rectal prolapse is also performed under general anesthesia, and requires a longer hospital stay than the treatment for rectocele and enterocele. The procedure may be performed through an abdominal incision in individuals healthy enough for surgery, and patients are often required to stay as long as one week in the hospital to make sure there are no signs of infection. Those who are unable to undergo general anesthesia may have the repair performed through the perineum, though the chances for recurrence are higher than with abdominal surgery. In rare cases where surgery is not an option, the sphincter may be closed manually by the doctor using a small wire inserted into the rectum.
AS FEATURED ON:
AS FEATURED ON:














Discuss this Article
Post your comments