At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What is Skin Atrophy?
Skin atrophy is a thinning of the upper layers of skin, causing them to be more fragile and prone to tears and ulcerations. Underlying structures like blood vessels, bone, and fat can also become more pronounced and visible. People can develop this condition for a number of reasons, but the two most common are aging and topical steroids, both of which lead to thinning of the skin over time.
People with thinned skin may find that it creates an unpleasant appearance from an aesthetic perspective, because of the more visible veins and fat underneath. It can also create health problems. The skin is supposed to protect the inside of the body and when it is thin, it can tear easily, allowing infectious organisms inside. This can lead to disease, as well as problems like rashes, fungal growths on the skin, and so forth.

When skin atrophy is caused by steroids, stopping the medication can give the skin time to recover, although it can take a year or more to regain full thickness. Medications to increase production of skin cells can sometimes be helpful for speeding this process along. In older adults, skin atrophy is hard to treat. Medications may be useful in some cases. Using moisturizer to keep the skin flexible and hydrated is also beneficial, as it makes the skin harder to damage. Patients also need to be alert to early signs of skin problems so they can take appropriate action.

Early warning signs of skin atrophy include tension or tightness in the skin, pain, pitting, dryness and a papery texture or appearance, and increased visibility of blood vessels in the skin. The face is often the first place people notice the problem, because the skin there is more sensitive and also more visible. Patients can meet with a dermatologist to explore possible causes and talk about potential treatment options, including medications or changes to a skincare regimen like using gentler soaps and being more aggressive about moisturizing the skin.

Patients with skin atrophy should make sure other care providers are aware of the problem. The use of some medications may be contraindicated in patients with thinning skin, and doctors also want to be careful about things like adhesives on bandages, antimicrobial soaps and swabs, and other things they may use in contact with the patient's skin. In a patient with thin skin on the chest, for example, electrodes and leads for an electrocardiograph test may pull at the skin and cause cuts and tearing.
AS FEATURED ON:
AS FEATURED ON:













Discussion Comments
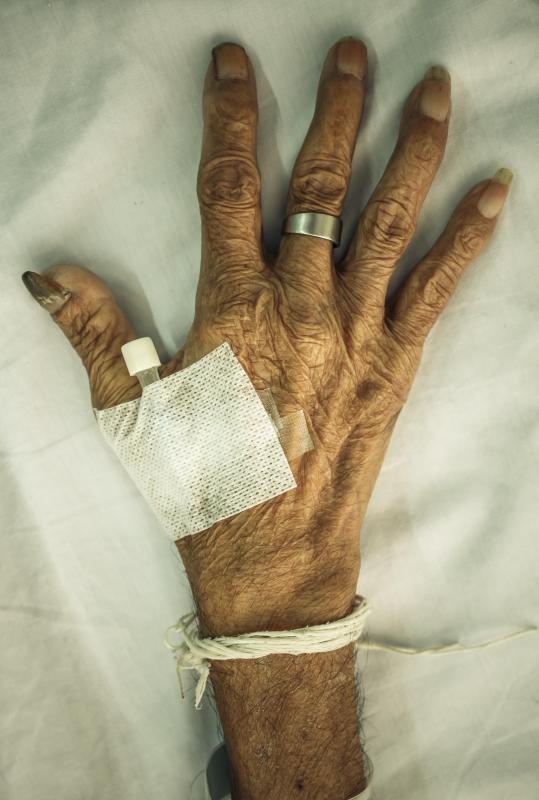
My grandmother's hands are the picture of skin atrophy. I can see her veins and tendons so clearly, and they almost look like skeleton hands!
She had a puppy, but I had to take it because every time it scratched playfully at her hands, it made her bleed. Her skin tore so easily, and it took a long time for the blood to clot because of her paper thin skin.
I'm glad that skin atrophy is only a side effect of topical corticosteroids. I have to take oral steroids and steroid injections when I get sick, and I would hate for the skin all over my body to be affected by this.
I seem to be prone to getting strep throat and bronchitis. These are two things that my doctor always gives me steroids for, and though I know that there are bad side effects potentially associated with these, too, they aren't as bad as skin atrophy.
Atrophy of the skin is something that I fear. I know that if I live long enough, it will inevitably happen, and there doesn't seem to be much I can do about it.
However, I've heard that if you use body lotion and face moisturizer, you can stave it off awhile longer. My mother-in-law is fifty and looks like she's thirty-five, and she says that her secret is always moisturizing after a shower.
I suspect that in her case, good genes may be a factor, but that won't stop me from trying. I'm in my thirties now, and I've already started using anti-aging moisturizer on my face and lotion everywhere else. I moisturize my face in the morning after washing it and at night after a shower.
It always scared me that one of the side effects of cortisone was thinning of the skin. I suppose that's why the label says not to use it on large areas of skin.
I have to use cortisone cream to treat my poison ivy sometimes, because it is the only thing that clears up the rash. I only use it directly on top of the bumps, because I'm so scared that my skin might start to disappear!
Post your comments