At WiseGEEK, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What is Sialadenitis?
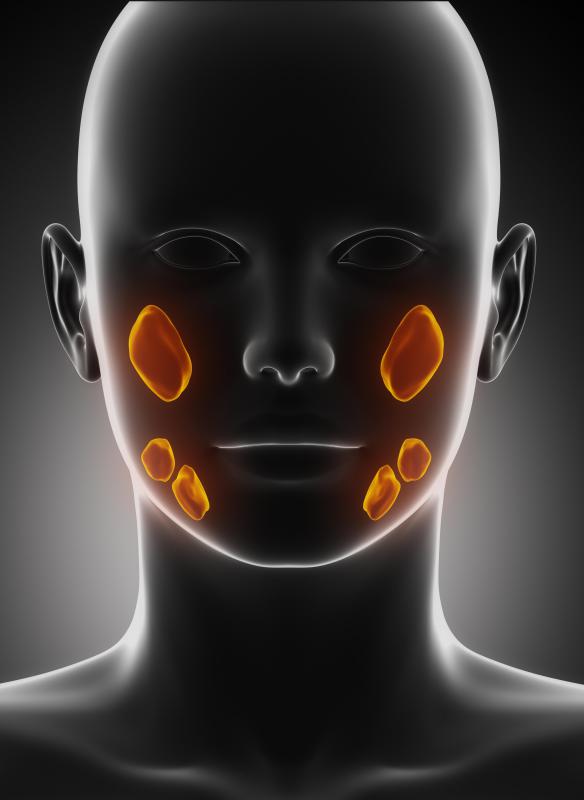
Sialadenitis refers to acute or chronic inflammation of one or more salivary glands in the face. Most instances of sialadenitis are the result of bacterial or viral infections, though adverse drug reactions, congenital deformities, and autoimmune disorders can also cause salivary gland problems. Common symptoms include facial pain and swelling, dry mouth, and mild fever. Treatment for sialadenitis depends on the underlying causes and may include oral antibiotics, warm compresses, or surgical intervention.
The majority of acute sialadenitis cases are caused by bacteria, especially Staphylococcus infections. Poor oral hygiene is a major risk factor for bacterial infection. Viral infections such as the mumps, herpes, and HIV can also lead to sudden salivary gland inflammation. Chronic sialadenitis is often the result of salivary stones, hard deposits of calcium and other minerals that build up in the glands and cause blockages. Less commonly, a person can experience this condition as a result of an immune system reaction to drugs administered to treat other glandular conditions.

Symptoms of sialadenitis can vary depending on the severity of an infection. Most people experience some degree of pain when opening their mouths, noticeable facial swelling, and skin redness. An individual may have an usually dry mouth or a persistent bad taste. In addition, fever is common with acute infections. An infected gland that is left untreated may develop a pus-filled abscess that can drain into the mouth and throat.

A dentist or primary care physician can usually diagnose a salivary gland infection by asking about symptoms, feeling the face, and testing saliva and blood for the presence of bacteria. A patient may be referred to a specialist for further testing if a diagnosis cannot be confirmed. Computerized tomography scans of the head and neck are often taken to determine the severity of swelling and look for possible signs of cancer.

Once the condition has been diagnosed, a specialist can determine the best course of treatment. Most bacterial infections can be relieved by taking antibiotics and practicing good oral hygiene. Medications are also available to lessen the severity of symptoms caused by viral infections. A patient may be instructed to massage his or her cheeks and apply a warm compress to help lessen swelling and pain.
A severe infection may require hospitalization and surgery to correct. A surgeon can aspirate the abscess by inserting a needle into the gland and extracting the pus. Rarely, an infection can necessitate surgical removal of part or all of a salivary gland. A patient who undergoes surgery is typically prescribed antibiotics and scheduled for follow-up visits to ensure the condition has resolved. With smart hygiene practice and regular trips to the dentist, most people do not experience recurring problems.
AS FEATURED ON:
AS FEATURED ON:












Discussion Comments
oops, sorry. It's not the submandibular gland but the lower part of the parotid. Inflammation started about seven years ago. anon136201
I have been diagnosed with sialadenitis. Symptoms are swollen submandibular gland, no pain, no redness. The needle aspire shows cell component consisting of clear cytoplasmic foamy, acinar cells with round nuclei arranged in small groups, few ductal cells in a background with lymphocytes and some polymorphonuclear neutrophils. No malignity. Antibiotic and anti-inflammatory medication don't work. Any suggestions on what this could be?
Post your comments