At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What Is Renal Parenchymal Disease?
Renal parenchymal disease includes maladies that damage the outermost internal region of the kidney where filtration and urine formation occur. Autoimmune disorders, medical conditions, or obstructions may all contribute to this disease. Lupus, bacterial infections, diabetes and high blood pressure, along with kidney stones can traumatize delicate tissue, causing scarring and possibly leading to eventual kidney failure. Managing systemic disease processes, however, may prevent kidney damage and failure from occurring.
Millions of nephrons lie within the renal parenchymal area of each kidney. The nephrons contain arterioles, or small blood vessels, known as glomeruli, that are surrounded by tubules. The glomeruli receive oxygen rich blood that contain excess electrolytes, salts, and water and transport the unnecessary blood products and water to the renal tubules. The tubules pass through the renal medulla, or the center of the kidney, into another system of tubules that combine and empty into the ureter.

Studies estimate that up to 50% of patients diagnosed with lupus erythematosus experience a renal parenchymal disease known as lupus nephritis. Lupus causes abnormal antibody production in the body, and these malfunctioning antibodies attack healthy cells, including those within the nephrons. The kidney's normal filtering processes are diminished when cell damage in the parenchymal tissue occurs. The disease might also produce inflammation of the kidney, adding pressure to damaged glomeruli.

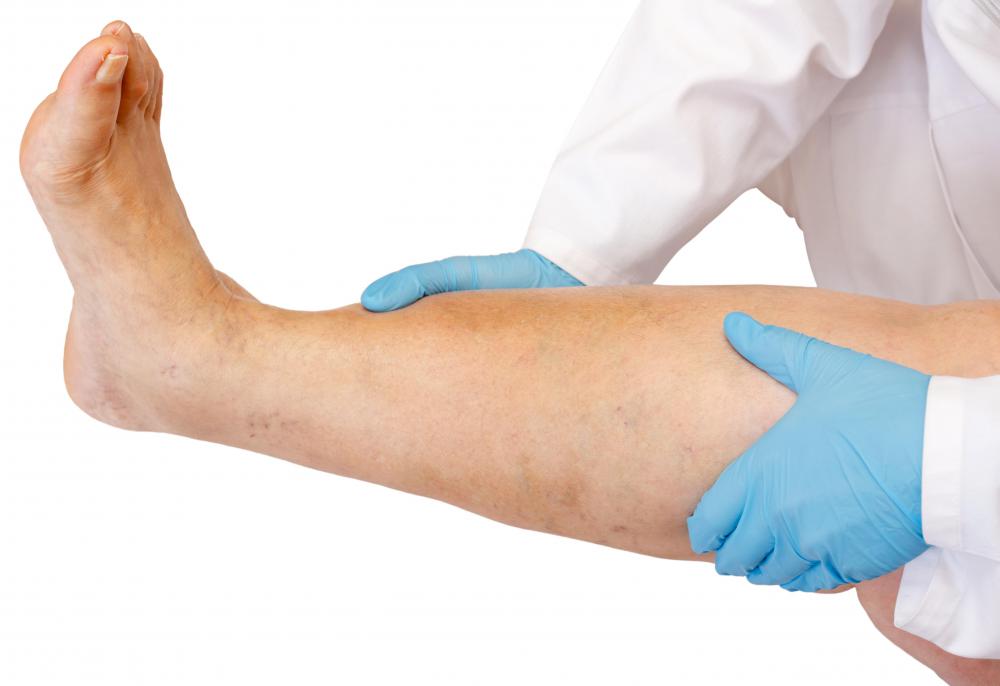
Symptoms of lupus nephritis include swelling in the feet, legs, and around the eyes. Patients may excrete urine that appears foamy or bloody. Inadequate filtering and excess fluid also cause increased blood pressure. Blood tests evaluate the efficiency of the filtering process and ultrasound imaging reveals abnormal kidney tissue. Treatment may include glucocorticoids and chemotherapeutic agents to reduce overall inflammation.

Uncontrolled diabetes may eventually lead to renal parenchymal disease and subsequent kidney failure. The flood of sugar-laden blood in the glomeruli puts increased stress on the filtering system and increases pressure within the delicate arterioles. The strain of continuously ridding the body of sugar diminishes filtering ability and eventually causes permanent damage. Protein spills into the urine instead of staying in the blood and sugar also enters the urine. Renal insufficiency contributes to hypertension, but hypertension can also cause renal problems.

Excess body fluids trigger renin/angiotensin release and subsequent response from the sympathetic nervous system to constrict blood vessels, forcing more blood to the kidneys. Renal parenchymal disease takes place when this constriction forces fluid through fragile glomeruli and other capillaries, causing cellular damage to vessel linings. During the reparative process, scarring occurs, and vessels become thickened and stiff. Without a permeable surface, glomeruli filtration is diminished.

Cellular and tissue damage can also occur when an patient has kidney stones. Uric acid and calcium crystals combine with oxalate to form stones of various sizes and shapes. Bacterial infections initiate increased enzyme, ammonia, and other chemical production, which may produce a by-product known as struvite stones. Besides inflammation and swelling, which contribute to decreased filtration, the foreign objects may tear vessels and tissues. Scar tissue forms, inhibiting proper kidney function and contributing to renal parenchymal disease.
AS FEATURED ON:
AS FEATURED ON:
















Discuss this Article
Post your comments