At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What is Methemoglobin?
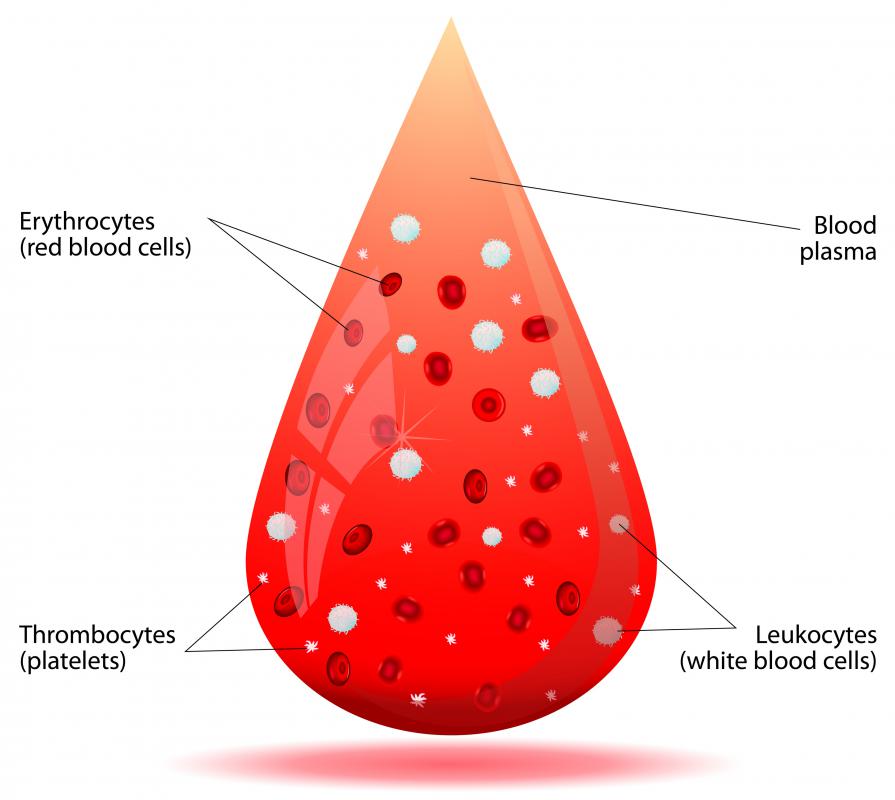
An altered form of hemoglobin, methemoglobin is the component of the blood responsible for carrying oxygen around the body. It is always present in the blood in small quantities, but when the levels increase and begin to replace the vital hemoglobin, the body falls into a state of cyanosis. This is because methemoglobin is useless for carrying oxygen around the body. It is made when the ferrous iron present in hemoglobin is oxidized into ferric iron. Methemoglobinemia is the condition associated with excessive amounts of methemoglobin in the body.
Methemoglobin usually makes up less than one percent of the body’s red blood cells. This doesn’t cause any medical issues, because there is still a sufficient amount of hemoglobin in the blood to supply the body with oxygen. When the body’s levels rise to above one percent, not enough oxygen can get around the body and the result is methemoglobinemia, a form of anemia. Minor cases of this often go undiagnosed because it only presents with symptoms such as skin and blood color changes. The skin goes through cyanosis, turning a grayish blue, and the blood can turn a shade of brown.

Methemoglobinemia can be caused by a genetic condition or exposure to environmental toxins. The genetic conditions that can cause excess methemoglobin to be produced in the red blood cells include Hemoglobin H disease and deficiency of methemoglobin reductase. Hemoglobin H disease is common throughout China, Thailand, Vietnam and other countries in Southeast Asia. Methemoglobin reductase is required to break down methemoglobins into the common oxyhemoglobins. Exposure to chemicals such as nitrates and chlorates can also result in excess methemoglobin in the blood.

The levels of methemoglobin in the blood affect the symptoms the condition presents with. If there is between 10 and 25 percent in the blood, cyanosis is the primary symptom. As levels increase to 35 to 40 percent, the resulting oxygen deficiency leads to shortness of breath and headache. If levels become more critical, at over 60 percent, the affected patient will fall into a stupor and begin to show signs of lethargy. Any level over 70 percent is likely to result in death.

Methylene blue is generally used to treat methemoglobinemia, at dosages of 1 to 2 mg diluted in a saline solution and administered intravenously. Blood transfusion is another option for treatment, usually only considered when patients do not respond to methylene blue. If the excess methemoglobin is being caused by an environmental agent or toxin, it must be removed as soon as possible.
AS FEATURED ON:
AS FEATURED ON:















Discuss this Article
Post your comments