At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What Is Hypoplastic Right Heart Syndrome?
Hypoplastic right heart syndrome is a congenital heart defect in which the right ventricle of the heart fails to grow and develop appropriately. The underdeveloped ventricle cannot contain the proper amount of blood pumped from the right atrium, and because the muscle's structure is poor, additional problems are encountered as the heart attempts to pump blood to the pulmonary valve for transfer to the lungs. This condition needs immediate and emergency treatment, as the heart begins to fail almost immediately after birth. An inadequate blood supply to the lungs means a poor return of oxygenated blood to the body, and the muscle in the ventricle will exhaust easily.
Babies born with hypoplastic right heart syndrome tend to be cyanotic, turning blue shortly after birth. If the condition has not been diagnosed earlier, the obstetrician or pediatrician will hear a discernible murmur with a stethoscope. An echocardiogram can then confirm diagnosis. Some radiologists notice a significant size difference in the ventricles during routine prenatal ultrasounds. Unfortunately, not all do, and fetal echocardiograms are not routine, though they are significantly less invasive than other routine procedures, like amniocenteses.

If this heart defect is diagnosed in a fetus, the parents are referred to a hospital with a pediatric cardiology and pediatric cardiothoracic surgical team. It is best if the baby is born at this Level 3 hospital, so cardiologists are on hand to assess and immediately treat the newborn. If the mother does not live close to a Level 3 hospital, early arrangements can be made for either an induced delivery or a Caesarian, if the mother cannot have a vaginal birth.

As with most heart problems, a hypoplastic ventricle does not pose problems to the fetus, but after birth, when the baby’s body must provide its own oxygen, problems begin almost immediately. If the baby is born in a hospital that cannot support immediate care, the infant is transferred immediately to a Level 3 hospital. Pregnant women who do not live close to a Level 3 hospital, especially those who plan a home birth, should request a fetal echocardiogram, particularly if there is any family history of heart defects.

There is no way to repair a small right ventricle, though its effects can be addressed. Surgeons rely on the Fontan procedure to bypass the right ventricle. The Fontan is split into two procedures, the Glenn shunt and the Fontan completion; early Fontans were performed in one step, but splitting the procedure is more successful. In the first few days of life, the baby will also be given a temporary shunt, called a Blalock-Taussig shunt, that provides a temporary way for blood to get to the lungs.

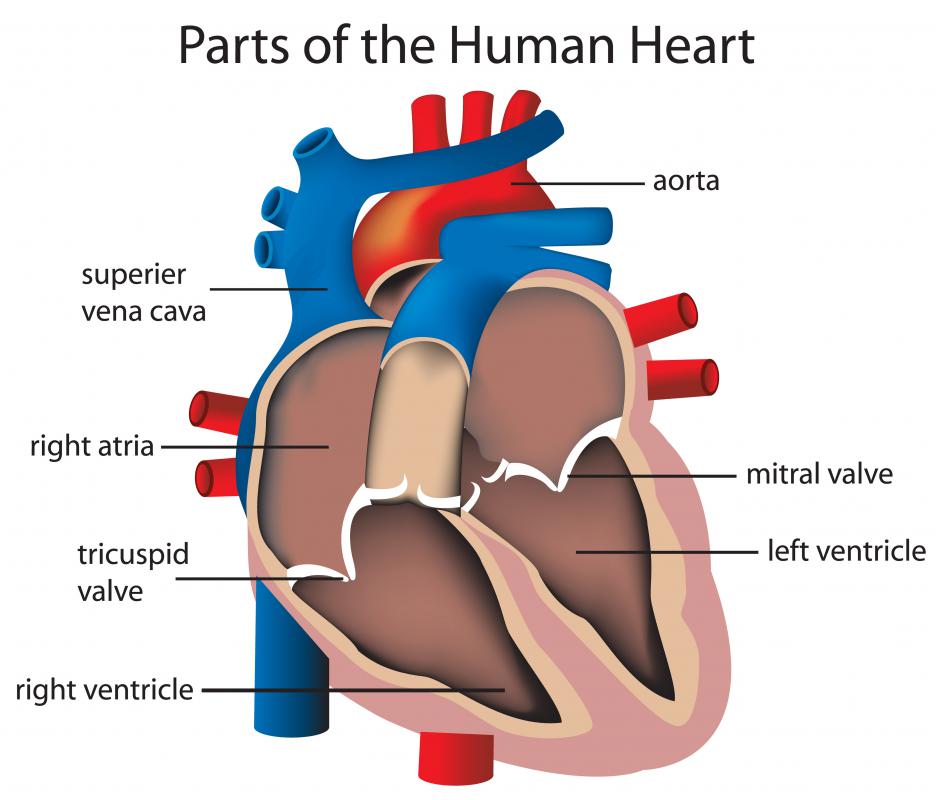
In about three months, the child undergoes the Glenn shunt, in which the superior vena cava is attached to the pulmonary arteries. Sometime in the next three to five years, the surgeons will complete the Fontan, which connects the inferior vena cava to the superior vena cava through an intra-cardiac baffle or tunnel, or through an extra-cardiac shunt. The result is complete bypass of the right ventricle, so blood flows back from the body directly into the lungs.
Many surgeons now prefer the extra-cardiac shunt because the Fontan completion can thereby be performed on a warm, beating heart. It does not require heart lung bypass and has a lower risk of inducing arrhythmias. Some surgeons still prefer the older intra-cardiac baffle, however, and parents should ask which type of Fontan surgeons tend to employ.
Most surgeons now predict a survival rate of 15 to 30 years post-Fontan. This does not mean that the child will die at this time, however, and when heart function begins to deteriorate, the individual will be listed for transplant. Some parents opt immediately for transplantation after birth instead of the Fontan. Other parents feel that transplantation technology still needs work, and prefer to buy time for this technology to improve by choosing the Fontan route.
The outlook for children with hypoplastic right heart syndrome is better now than it has ever been, and the improvements in care and surgeries have made an enormous change. This birth defect used to be considered almost certainly fatal, but now many children survive the initial surgeries and are able to pursue active and purposeful lives.
Frequently Asked Questions
What is Hypoplastic Right Heart Syndrome?
Hypoplastic Right Heart Syndrome (HRHS) is a congenital heart condition that impedes normal development of the right side of the heart, causing insufficient oxygenated blood flow in the body due to underdeveloped right ventricle, right atrium, and pulmonary valve.
What are the causes of Hypoplastic Right Heart Syndrome?
It is usually caused by a combination of genetic and environmental factors and may be more prevalent in infants with family history of congenital heart issues or exposure to certain medications or toxins during pregnancy.
What are the symptoms of Hypoplastic Right Heart Syndrome?
Common signs and symptoms of HRHS include shortness of breath, fatigue, slow growth, increased heart rate, cyanosis (bluish skin and nail discoloration due to lack of oxygen), heart murmur, and swelling in the legs and abdomen.
How is Hypoplastic Right Heart Syndrome diagnosed?
Diagnosis of HRHS is usually conducted prenatally or shortly after birth using physical exams, chest X-rays, echocardiograms, cardiac MRI scans, and other tests.
How is Hypoplastic Right Heart Syndrome treated?
Treatment for HRHS is dependent on the severity of the condition and its associated symptoms. Medications may be used to manage symptoms, surgery may be used to repair or reconstruct the affected heart structures, and lifestyle changes such as a low-salt diet and oxygen therapy may also be implemented. In severe cases, heart transplant may be necessary.
AS FEATURED ON:
AS FEATURED ON:











Discussion Comments
I am a 21 year old woman who had open heart surgery at 4 days old to fix Hypoplastic right Heart Syndrome. I am successfully working my way through college, engaged to the love of my life and planning a very long future ahead of me. I keep up with my cardiologist each year and have never had any surgeries after the first, nor have I had any issues. I played softball competitively for 12 years and exercise regularly (though I cannot run long distances and do get winded semi-easily). HRHS is not a death sentence for a baby as long as you have competent doctors around you and you follow their instructions.
I'm 22 weeks pregnant and just found out that my baby girl has HRHS. We did the amnio test immediately and are anxiously waiting for the results. After I spend the entire day being told all of the horrible things that could come from this and crying the entire day, I still chose to not abort because I want to give her a chance to fight.
After reading all of these stories, I couldn't help but cry some more but with happy tears that she really does have a shot at this and me choosing not to abort was the right choice after all. I can't thank you all enough for giving me and my boyfriend hope for our precious angel.
My son was born with a undiagnosed Hypoplastic right heart syndrome. He lived for 30 minutes and then passed away as the hospital was not expecting this complication. I keep wondering if the ultrasound should have picked this up so we could have prepared. Our family is so sad.
@anon119081, 26 year old female: Can you please tell me which surgeries you had? My daughter is a two year old version of you! You're an inspiration.
My son is 25 years old (born with HRHS, ASD, VSD, and Pulm. Atresia) He had surgery after birth, at 3 years, and at 13 years. He has a pacemaker, and takes a mild heart medication for preventing clots. He cannot play organized contact sports, because of the chest surgeries, but got away with Little League Baseball wearing a chest protector. He was on the small side in his physical growth, but has been able to keep up with his peers, running, swimming, etc.
In college he even played intramural soccer and basketball. He is checked by cardiologists once a year (Texas Children's Hospital). We are told that "someday" he will probably require a heart transplant, but I don't think he lives in dread of that day. Overall, he lives quite a normal and happy life. Our family is truly blessed!
My son was born with right heart ventricle problems. He made it through surgery really well. He is only a month old. I was told by the doctor since he needs constant care, that I would not be able to raise him, since I have another son who is autistic. So to see him survive was amazing. He loves to eat. But he lives with his father, and I cannot see him.
Yesterday, they told me that my baby girl (I'm 23 weeks pregnant) have the HRHS and I was devastated, and today I talked to the geneticist, and was told a lot of things that put me in worse emotional stress.
Now, after reading all this, I'm having faith that it's going yo be all right. I have a two year old boy and he is super fine! I hope my baby girl, even with the condition can be as strong as he is. They are my angels!
My brother has HRHS and is still going strong.
I am 28 weeks pregnant, and during the sonography, it was found that the baby has a small, underdeveloped right ventricle, right atrium, an underdeveloped rvot with pulmonary artery hypoplasia, the tricuspid valve appears atretic and the Lv,la,lvot appears normal. The diagnosis is hypoplastic right heart syndrome.
Please tell me whether the baby will survive after birth and needs to be done for the birth.
I have a pregnancy of 28 weeks & during sonography it is found that a baby has a small underdeveloped rt ventricle, rt atrium.Underdeveloped rvot with pulmonary artery hypoplasia. Tricuspid valve appears atretic. Lv,la,lvot appears normal. P/o hypoplastic rt heart syndrome.
Please convey whether the baby would survive after birth & what is need to be done
My granddaughter is 9 years old. and a CHOP baby for life! She is on a competition cheer team, a flier no less, plays basketball, bikes, dances, swims and runs around like any other 9 year old, and has HRHS and three or four other defects as well. However, with God, awesome parents and a mighty spirit, all things are possible.
She will be the one to introduce the one of the scientific breakthroughs. It's on her "to do" list.
Thank you all for the great encouragement in the posts. My wife and I have been told about our soon to be born child having a hypoplastic right ventricle with ASD and hypoplastic pulmonary artery. We don't know what to do. We are very confused about the quality of life of our child will have after the surgeries, plus we're not sure about the quality of surgeons in our part of the world.
We want to give the child a fighting chance, but wonder if we are being selfish in bringing a baby that will have a very tough life ahead. Please advise.
There is hope! For all those parents and their families who are terrified of what the diagnosis of HRHS can mean.
My son and daughter-in-law found out when they were 21 weeks pregnant that my granddaughter had HRHS. They were given the pro and cons and chose to give her every possible shot at life. She was born a month early, strong and fighting. Her shunt was placed 20 minutes after delivery and the months that proceeded it were scary but allowed us to fall deeply in love with this precious angel. She just completed her Glenn procedure and is doing beautifully. Now this process was wracked with stress and exhaustion but to see her now it was worth everything. God graced our family with her and I thank him for her every day.
I was born with hypolastic right heart syndrome. I had three surgeries at three days, nine months and a year and a half. I am now 20. I see a heart doctor every year.
My son is three months old, he was born with dextracardic single ventricle, and had undergone BT shunt surgery, and also undergone Malrotation TAPVD also, now we don't want to proceed for further surgeries. How many months can a baby survive with this shunt? Can you please let us know.
I'm 20 weeks pregnant and my baby boy has been diagnosed today with HRHS. I'm mot going to terminate my pregnancy; he deserves a chance to survive. I have faith in today's advanced care for those problems and I have faith in Christ.
My daughter is 27 months old and was diagnosed with HRHS when I was 16 weeks pregnant. What a shock this was, questioning what to do. Can I handle this or not? This condition is not picked up with genetic studies. It is not a genetic disorder. The chromosomes were normal, and I also have a four year old without any problems.
She had a BT shunt at two weeks old and the Glenn Shunt at five months old. She is expected to have the fontan at about four years old. She is thriving, and you would never know anything is different about her, except her beauty scars on her chest.
She amazes me; nothing slows her down, and she's a feisty one! I never thought I could handle what this diagnosis involved. But I wouldn't trade all the difficult times for anything. For anyone out there questioning, you were chosen, you will be strong enough, and you will make it through it, and will appreciate life, and be a stronger person in the end! You will enjoy the hugs and kisses from these kids who need you, who have brought them into this world. Fight for these beautiful babies!
I have a question about hearing related issues. Are there any reports of hearing loss related to HPRH?
i have had two five-month pregnancies diagnosed with HRHS. Doctors don't know the exact recurrence rate, but it's somewhere between a 25 percent and 75 percent chance of it happening again.
I have a 5 1/2 year old daughter born with Hypoplastic Right Ventricle. She has gone through three surgeries (PA band at one month old, Glenn at five months old and Fontan at just shy of three years old). She is a healthy active little girl! She does dance, and runs and plays. she does have limitations but she knows what they are.
I also have two other beautiful girls, a three year old and a one year old who are healthy. They do not have any problems with their hearts. it isn't genetic!
my grandson was diagnosed with hypoplastic right heart syndrome in the womb at six months gestation, so for three months my daughter was worried as to whether or not he would survive.
He was born at a special unit in bristol in February and was strong at birth, so strong he didn't need oxygen at birth. He was and is an *amazing* little fella. His operation was planned for three months old and so the day came and we were all petrified we might lose him. However, he had two procedures performed: the glen shunt and the fontan procedure. This was a four hour op and seven days later, he was recovering well and will be allowed home soon!
These babies are stronger than we all assume and today's procedures are just fantastic, so for any parents with a baby with hypoplastic heart syndrome I'd like to say have faith the outlook is better than you think. Put your faith in the fantastic surgeons because they are absolutely brilliant!
My grandson was back to his old self just a week after the op and it's just fantastic his life has been saved, as have many others before him. Keep positive because the outlook is better than ever in 2011.
I hope this helps all parents/grand parents in this difficult situation because i know exactly how you feel, believe me. He will of course need another op at three to five years. However, he will be a lot stronger then and i believe he will breeze through that op as well. This op has been performed so many times its now been perfected to an almost 100 percent success rate.
My son Jackson was born three weeks early and suffered from HRHS, Tricuspid Atresia, VSD, Tetralogy of Fallot, and Pulmonary Stenosis. He was diagnosed as a fetus at five months. I was really scared and confused but we had the most amazing ped. cardiologist who took care of him before and after his birth.
Jackson is nearly a year old. He had the BT Shunt at four days old and the Glenn Procedure at six months. The only medicine he is on now is Lasix once per day. We follow up with the cardiologist regularly (we only have to go every three months now).
We were told that he would need the Fontan Procedure this August but now they are telling us that he is doing so well that we may be able to put it off for six months to a year. Jackson's oxygen levels are 88 to 92, depending on the level of activity he has done prior to spot testing. Thanks to Dr. Neill Videlefsky (Cardiologist) and Dr. Kirk Kanter (Surgeon at Egleston in Atlanta, GA) we have a very happy, active almost one year old.
My husband and I never expected to have another baby because we have 21 year old twins and a 16 year old son, but God gave us this special blessing and I wouldn't trade it for the world!
My daughter was born in 1992 with right hypoplastic heart. She is getting ready to graduate. She has done very well. She doesn't tolerate the cold well but other than that, you would not know she has a heart problem unless you see her scar.
She can't play sports but has rodeoed since the age of 5. She has actually won two world championships in pole-bending. She has also won many belt buckles and saddles. Through Christ all things are possible. It has been a quick 18 years.
My son was born in August with Hypoplastic Right Heart, VSD, ASD. He had the BT shunt and we are getting ready for the Glenn Shunt in the next few weeks. He is doing amazing and is a happy, beautiful baby.
The only problem we are having is that he isn't gaining weight because he gets really tired out with his feeds. They increased his calories to compensate for his lack of intake, and he is gaining weight again. It is very stressful at times, but I wouldn't have it any other way.
There is a reason we are picked to be parents to these special kids. Anyone can have a "normal" baby, but it takes someone who is blessed to handle ours.
My son was born with hypoplastic right heart. He was six and 1/2 weeks premature. I didn't find out till the next morning when the cardiologist called me. i was in one hospital and he was in another 25 minutes away. It was a horrible feeling to think your having a healthy baby and you find out something like that.
I had an amnio done mid pregnancy and it showed nothing. I know some kind of a chromosome combination is supposed to show if a baby has HPRH but my son didn't have those chromosomes.
He is six now and has been through all the surgeries and is the most active child i know. I would hope anyone would not get an abortion due to HPRH in your baby. But god is giving you a miracle and a challenge all at the same time. my son went to cardiology today and the echo showed everything is great and he is a healthy active boy. And the chances of the second child having this is slim to none. It's just something that happens and you have no control over it.
Hope this helps!
My daughter was diagnosed with Hypoplastic Right heart Syndrome when I was five months pregnant. They told me her prognosis was not good. I chose to continue with the pregnancy. I had her at 38 weeks. They misdiagnosed her! She ended up only having pulmonary atresia.
She is now 5 years old, completely healthy with no open heart surgery. The chances of having another baby with a congenital heart defect are less then one percent. Two years later I had a healthy baby boy.
I had a sister who had this disease. She died just three months short of two years old. she had many surgeries and none of them seemed to work. It was a very miserable year.
I am a 26 year old women who was born with situs iversus totalis, dextrocarida, tricuspid atresia, hypoplastic right ventricle and severe pulmonary stenosis. I have had five surgeries so far.
My mother was told that I was not going to live past 21 but here I am, alive and well. I can't do sports or any activity that increases my heart rate but that's OK -- at least I'm alive. I suffer from arrhythmias so I take medication for that. I still go to the doctor every six months but that is the price I pay for being born with a heart condition. I just make sure my heart is doing OK.
My son is now 15 years old, soon to be 16. He is a very active teenager. He was born with HRHS, Tricuspid Atresia and Transposition of the Great Arteries. He had his three surgeries, all before the age of 2. He just had a fourth surgery due to a clot in his inter-cardiac baffle, so they revised his fontan procedure and he now has an extra-cardiac shunt. Once again, he is back to being active and healthy. While he is limited in some sports, he lives a healthy active lifestyle.
To God be the glory! I'm 22 weeks pregnant and my baby been diagnosed with HRHS. I am so torn and confuse, I don't want to have an abortion and I don't know about putting a newborn through an open heart surgery. I have faith that maybe this is a test and that everything will be fine! All I can do is pray for direction.
My daughter is four years old with HRHS and AVSD. She had a PA banding at three months and the Glenn at nine months. She is doing great. She is very active, does dance and soccer. We recently went to the cardiologist and they said that her right ventricle is now growing and they are going to do a cath to see if the can reverse the Glenn and therefore have a normal heart.
I have HRHS and I'm a 25 year old woman. I am very active, go to the gym most days, unless I'm being lazy. I can tolerate more exercise than most of my friends who have normal hearts.
My son is 27 months old and had his third surgery (the fontan) two months ago. He's doing excellent and has tremendous energy. His oxygen is in the mid to high 90's which is what a normal person has. For those who have a baby with this disease, there is hope. We didn't know until about eight hours after his birth that anything was wrong - his birth was the best and worst day of my life. Seeing him now amazes me.
My baby girl was diagnosed when i was five months pregnant. she had hypoplastic right heart, and I had an abortion. Please tell me. I want to ask if my other babies will have the same disease of Hypoplastic right heart syndrome. Please respond to me.
My baby is diagnosed with hypoplastic right heart syndrome, pulmonary atresia with intact ventricular septum and also observed tricuspid valve regurgitation. Currently we are at 22 weeks of pregnancy. Please guide further based on prognosis and risk factors.
my baby girl was diagnosed when i was five months pregnant. she had hypoplastic right heart, I had her at 38 weeks after induced labor. she died six days later. It's the worst thing ever.
why did we get hypoplastic right heart syndrome in our unborn child? we even had amniocentesis to detect problems and it didn't get picked up.
Why, why, why, why? what a crappy day.
I have a four year old girl with hypolastic right heart syndrome who is doing really well. She struggles with exercise as she becomes very tired easily and has undergone three surgeries so far. she's a little fighter.
What are the three major surgeries to repair the heart? What are the risks of each one of the surgeries?
how can my 26 year old son die of hypoplastic right heart syndrome with no previous signs or diagnosis? That is what was out on his autopsy report.
I had a baby boy with Hypoplastic right heart syndrome, and he died before I went into labor. I want to ask If my other babies will have the same disease Hypoplastic righ heart syndrome. Please respond to me.
I don't think petroleum jelly should ever be used on a kid's nose. You may want to look into a nice safe moisturizer like Vitamin E instead.
Also, what does you doctor say about the nosebleeds? I'm curious if your son is on blood pressure medications that can cause chronic cough or if he's on anticoagulants? I could see even aspirin or coumadin causing nose bleeds, and certainly an bp medications or vasodilaters causing cough. If he's on both the two might be related.
also, has the pressure in his lungs been checked since the surgery, or has he had a chest x-ray to rule out pleural effusions?
My son is three and has had the Fontan completion, however he continues to battle with nosebleeds with a severe cough. I make sure his nose is moist with vaseline, he has a humidifier right next to his bed and I even try to count liquid input and output to make sure he is hydrated. What else can I do to stop these nose bleeds?
Post your comments