At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What is a Mumford Procedure?
The Mumford procedure, also known as distal clavical resection, is a surgical procedure that aims to relieve shoulder pain by removing a small part of the clavicle, or collar bone. Patients suffering from painful inflammation, swelling, or osteoarthritis in the acromioclavicular (AC) joint — where the end of the clavicle meets the shoulder — may elect to have this procedure, especially if alternative solutions like physical therapy and cortisone injections are unsuccessful. The surgery can be performed using an open or arthroscopic procedure, and typically requires eight to ten weeks recovery time.
Reasons to Have this Surgery

Surgeons usually perform this procedure when bone spurs develop on the collar bone, narrowing the AC joint and preventing it from moving smoothly. These spurs can be caused by arthritis or overuse. A condition called distal clavicular osteolysis or "weightlifter's shoulder" can develop in people who put a great deal of stress on this joint; in this condition, the end of the clavicle begins to break down. Removing the damaged end of the collar bone can help relieve pain and restore movement for many of these patients.

The Mumford procedure is a relatively common and simple surgery, and has a high success rate. Clinical studies show that, depending on the underlying problem and the type of surgery used, at least 75% - 90% of patients report good to excellent outcomes.
Before the Surgery
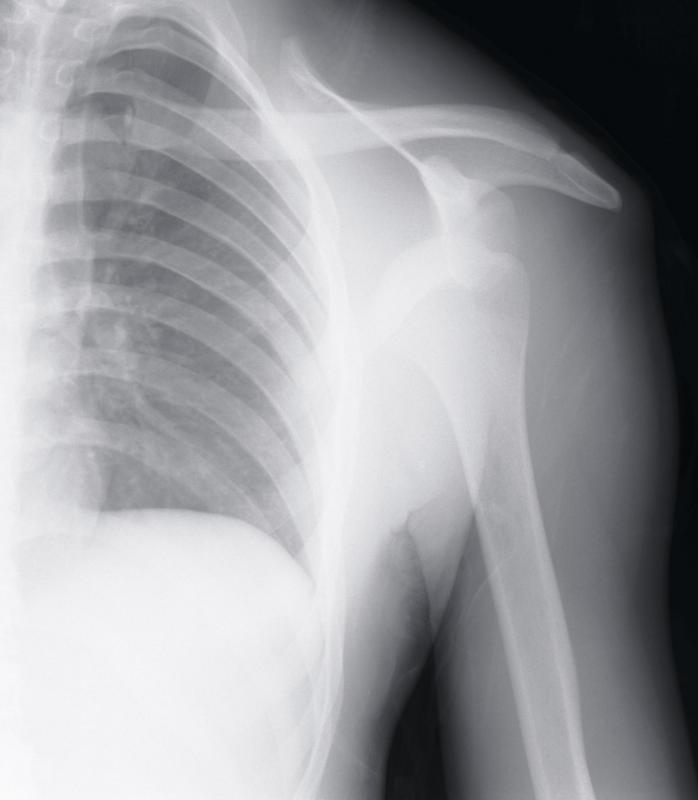
Before the Mumford procedure is recommended, a health care provider will evaluate the patient, feeling for swelling or tenderness in the AC joint and checking the patient's range of motion. A series of tests are performed to see if certain types of movement in the arm and shoulder will cause pain for the patient. This is followed by x-rays and magnetic resonance imaging (MRI) so that the health care provider can look for clear signs of bone spurs or other problems in the joint, and to help rule out alternate causes of pain.

Non-surgical treatment methods are nearly always recommended before a patient undergoes surgery to fix a problem with the AC joint. Such treatments can include icing and resting the shoulder, anti-inflammatory medications, corticosteroid injections, and physical therapy. Most health care providers recommend trying these methods for at least six months before considering surgical options.
Open Distal Clavicle Resection

During an open Mumford procedure using a direct approach, the patient may be given a sedative, along with general anesthesia or a regional interscalene block, which numbs the nerves in the shoulder and arm for up to 24 hours after the surgery. An incision is made on top of the AC joint, and the fibrous tissue, or fascia, over the joint is cut; it may also be necessary to release the shoulder muscles from the bone. A surgical saw is used to cut off about 0.4 to 0.8 inches (1 to 2 centimeters) or less of bone off the end of the clavicle. Pieces of the bone are removed and the tissue and skin are sutured back together.

In the indirect approach, the surgeon performs the procedure from below the joint rather than above. Many of the same steps are performed in this approach, although the bursa — a small fluid-filled sac that cushions the joint — is typically removed. The indirect approach is often preferred when other surgical procedures, such as a rotator cuff repair, are also being performed.
Arthroscopic Distal Clavicle Resection

Although the original Mumford procedure was an open surgery, advances have made arthroscopic techniques increasingly popular. As with open surgery, arthroscopic procedures can be performed using both direct and indirect approaches. In this type of surgery, several small incisions are made in the shoulder, and a camera and the surgical instruments are inserted into the joint. Unlike with the open procedure, it is typically not necessary to release the muscles to perform this type of surgery. The covering of the joint, known as the joint capsule, is removed and a surgical burr is used to shave off a portion of the clavicle.
Recovery
Both the open surgery and the arthroscopic surgery can be done on an outpatient basis, although in some cases, the patient may be required to stay overnight. The surgery itself typically takes one to two hours, the patient may require another two hours for the anesthesia to wear off. How long it takes for a patient to recover from the surgery itself will depend on which type of procedure was used and the body's own healing speed, but people who have arthroscopic surgeries usually recover faster. The incision in the skin and fascia and the release of the muscles in the open surgery will take longer to heal than the smaller incisions made during the arthroscopic procedure.
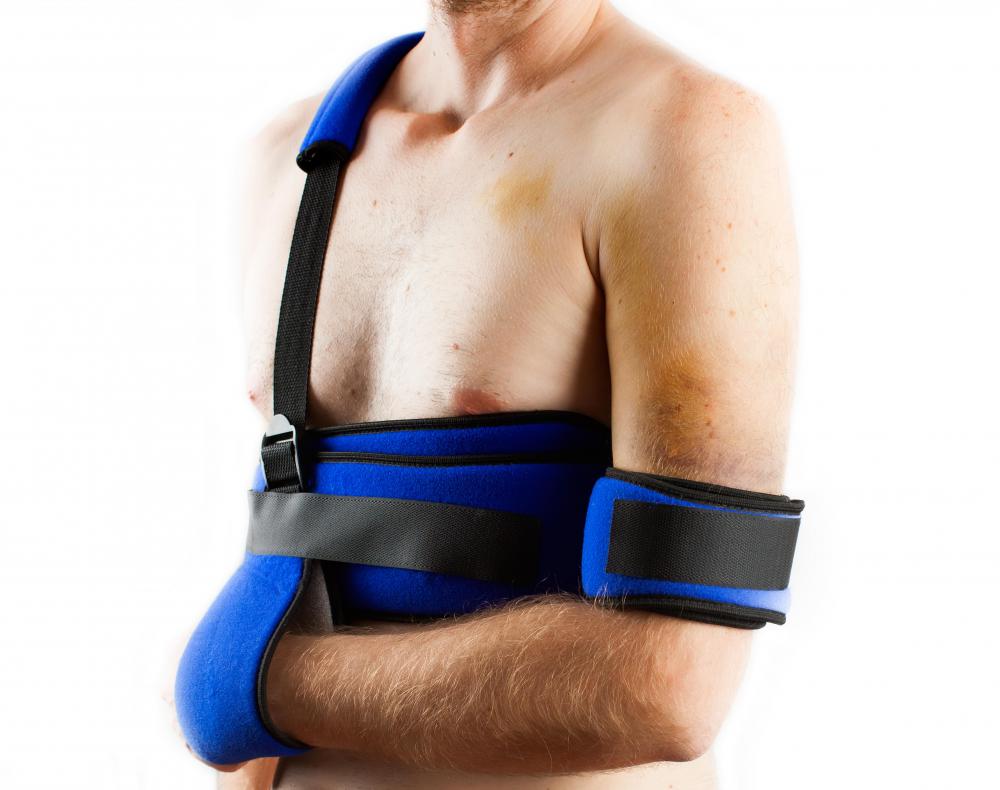
The patient will need to rest the shoulder and manage any pain and swelling with ice and medication for the first few days after the Mumford procedure. For the first day or two, the arm is typically immobilized in a sling, and any movement should be kept to a minimum. The bandages can often be removed after about two days with an arthroscopic procedure and a week after open surgery.
After a few days, light or passive arm movement may be recommended, and the patient can stop wearing the sling if doing so does not cause pain. After the first week, the patient may begin light physical therapy and range of motion exercises; even while wearing a sling, moving the fingers and hand can help with circulation. It often takes about three weeks for the patient to regain normal use of the shoulder and arm. Sports and other more strenuous physical activities should usually not be performed for eight to ten weeks after the surgery. The patient is advised to proceed with therapy slowly and report any pain to his or her physician.
Possible Complications
Complications from this surgery are generally minor and rarely occur, regardless of the procedure used. The most common complication is joint tenderness, along with stiffness and some minor loss of elevation. Some patients experience weakness in the shoulder and arm, particularly after the open procedure. The ligaments around the joint can be damaged during surgery, leading to shoulder instability. Infection in the joint is also possible.
In some cases, the surgeon may not remove enough of the bone during the procedure, so the patient may still experience long-term pain. It is also possible that problems with the AC joint were not the only causes of pain in the shoulder, so the surgery may not solve the underlying condition.
AS FEATURED ON:
AS FEATURED ON:












Discussion Comments
Just had this surgery three weeks ago. Had a nerve blocker and a pain pump which lasted two days. Still had some pain so took pain pills for two to three days ans then just had soreness and discomfort. Made up two weeks worth of meals ahead of time. You will need pull-on pants and a button shirt or a loose t-shirt, which I wore. It's hard to pull anything over your head. Hard to do your hair because you are doing everything with one hand. Make sure you do a lot of icing. I did have some help during the first week, but still could do most things by myself. I slept in a lazy boy the first two weeks. This was more comfortable than my bed and was recommended by a friend.
I had this procedure done two weeks ago and was feeling good overall. However, in the last three days I can no longer reach into my back pocket and am getting massive pain in front of my shoulder down the tricep. This is the same pain that was associated with my torn rotator cuff surgery a year ago. Would this be considered normal or should I contact the doctor now rather than wait until my next appointment in a week?
I had this surgery in a military hospital 14 years ago and the pain never went away. Over the last two months it has gotten worse. I saw a shoulder specialist today and the xray shows where the end was cut but the bone was not taken out. It sits right on top of the joint. It's a simple surgery now I guess, but thought removing the bone that's cut off is Mumford 101?
I'm a 60 year old woman, healthy and active, but gave up swimming seven years ago due to shoulder pain.
I finally decided to have surgery after several rounds of cortisone shots and PT. I had arthroscopic subacromial decompression and distal clavicle resection on my right shoulder in April 2012. I could not feed myself with my right hand for two weeks. I could not drive for three and a half weeks. I needed to take Percocet for pain for the first 10 days.
I was in a sling, but doing the few little exercises they tell you to do, for nine days. I started PT on day 11. Some people progress faster than I did, and others more slowly.
By week 4 I could do all self care myself. I still can't actively raise my arm straight up or out to the side myself, but, I am assured that will come. I would say anyone having this surgery should plan on having help at home for at least a week and a half to two weeks. Also, my PT says I could have started PT sooner. I will do this if I have my other shoulder done.
I had the open mumford procedure back in 2003. Thank God! The first three weeks post op, I kept asking myself why I went through it since the physical therapy was complete torture, but today, I am so happy I did! I am back to weight lifting and actually have more range of motion in the shoulder that was operated on than I do the other.
Now I'm going through a slight impingement in that shoulder, but so far it's doing well. If it gets to the point like my other shoulder did back in 2002 prior to the surgery, then I will definitely have this procedure done again.
How long does the operation take?
I had arthroscopic AC joint surgery. The AC joint is now painless, but I have significant pain in the rotator cup area. It feels as though it is in the top of the cup and in the bicep tendon. Isometric exercises are pain free, but reaching forward or out to the side can be very painful. What's is/has happened? What's the recovery?
@anamur: i just had this procedure done yesterday but with as an open surgery not arthroscopic. I am in extreme pain and would recommend someone be there with her as it is hard to do things one handed lol. You don't realize how much pressure and pulling you put on the shoulder doing simple things like adjusting yourself in bed. it's horrible. hope she does well.
@anamur-- The recovery stage can be experienced differently by different people, some recover more quickly than others after the arthroscopic shoulder surgery. So, even though I can't entirely predict how it will be for your aunt, I can tell you from experience that the first week after surgery can be a little challenging. I was able to do small things around the house, drive myself to the doctor etc. However, I did some preparation before the surgery and made sure I didn't have to worry about dinner or laundry after the surgery.
I would recommend that someone visit your aunt during this time to help her with physical therapy. She can go to the hospital for most of them, but she will need someone's help to do movements at home. Also, she should take time off from work because it will be too difficult and painful. She needs to rest as much as she can. I hope she gets well soon!
My aunt might have this surgery soon, she accidentally fell at her home and has been experiencing a lot of shoulder pain. After her MRI last week, the doctor recommended an arthroscopic shoulder surgery. My aunt is a bit anxious though, especially because there won't be anyone to help her during the recovery period. Can anyone who has had this surgery comment on how soon she can start using her arms and at least fix dinner for herself?
Post your comments