At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What Causes Uterus Scar Tissue?
Uterus scar tissue, also referred to as intrauterine adhesions, can be caused by several factors. Uterine scarring can be the result of trauma and the natural healing process. Surgery, dilation and curettage (D and C) procedures, and aggressive infection are also common causes.
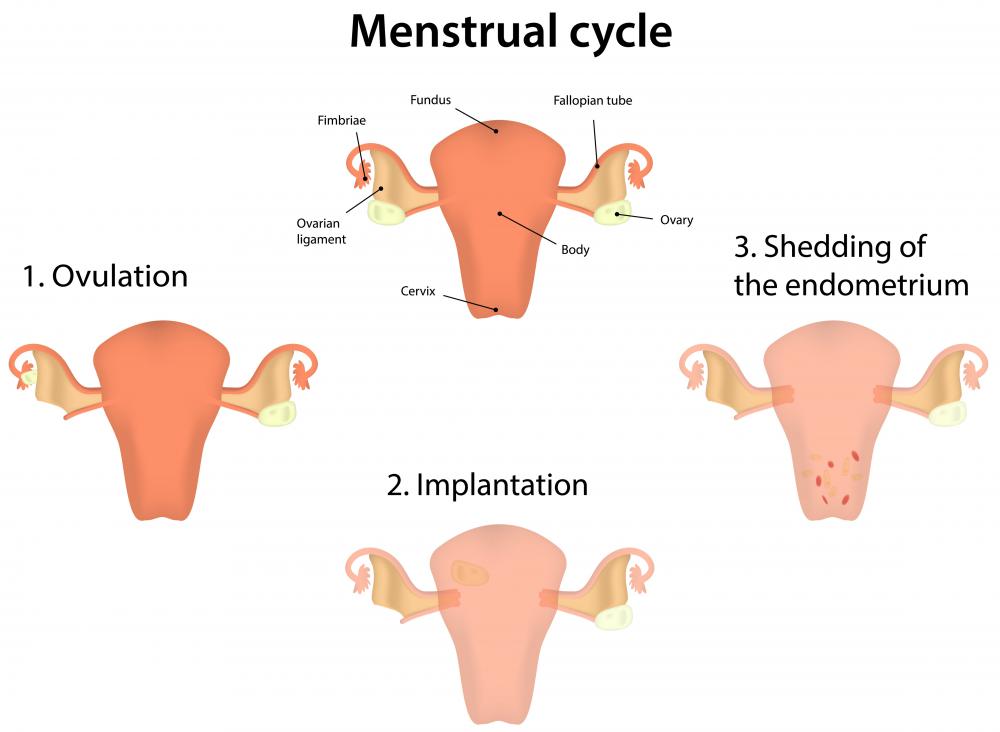
The endometrium is the term used for the uterine lining. It is comprised of two layers. The functional layer is the top portion of the endometrium that sheds during the menstrual cycle, and the basal layer is under the functional layer. Uterus scar tissue is found in this bottom layer.

When surgery is the cause of intrauterine adhesions, it is often related to a cesarean section or a procedure to remove fibroid tumors. Fibrosis is the condition where the uterine muscle develops non-cancerous tumors. These tumors are removed if they are abnormally large or impede fertility.
D & C procedures are often performed following a pregnancy miscarriage. During this procedure, the cervix is dilated and the uterine lining is scraped. Due to how this procedure is done, it is common to develop uterus scar tissue.

If serious infections occur in the uterus, the lining and the wall of the uterus can suffer damage. Minor infections do not generally cause damage to the uterus but some infections, such as those caused by sexually transmitted diseases, can result in scarring. In some cases, bladder or urinary tract infections can spread to the vagina and into the uterus. Other vaginal infections can also spread from the vagina into the uterus if they are left untreated.

Asherman’s syndrome (AS) is a condition that coincides with the presence of intrauterine adhesions. A woman with Asherman’s syndrome can have fibrous tissue in addition to the scars. Imaging results from a sonohysterography can detect the presence and extent of uterine scars.
Treatment of scar tissue in the uterus is an option when the scars cause problems such as infertility, pain, or abnormal bleeding. Removal of the scar tissue is possible with an operative hysteroscopy. This procedure involves a thin telescope with special attachments to carefully remove the scar tissue.

Medications can be prescribed that help prevent uterus scar tissue from returning. Sequential estrogen hormone therapy followed by progestin is often prescribed. These medications trigger the growth of the endometrium. In addition to medication in some cases, gel or mechanical barriers, such as stents, are used to prevent opposing walls from fusing together.
AS FEATURED ON:
AS FEATURED ON:













Discussion Comments
Can you tell me if there is an injection that will break down scar tissue from internal radiation after hysterectomy and bilateral salpingo-oophorectomy due to uterine cancer five years ago.
Can a low sex drive be caused by scar tissue?
@ElizaBennett - I chose a VBAC for similar reasons, although I don't think I'll have more than one more child at most. A friend of mine opted for elective repeat caesarean - her doctor recommended it and she just listened - and she mentioned that the first time she heard it mentioned that this surgery would take a little longer because of the scar tissue in her uterus from her previous section was *during the surgery.*
Of course, c-section isn't the only possible cause. A friend of mine had fibroid removal surgery in her 20s and developed adhesions. Basically, some of her other internal organs starting sticking to the scar tissue! She had to have a follow-up surgery to have everything put back in its proper place. It is possible that she could still carry a child, but they've decided not to try under the circumstances and are considering adoption, surrogacy, or living child-free as their options right now.
Adhesions and scar tissue don't get talked about enough, I think, as possible complications of caesarean births - especially repeated c-section deliveries.
My first baby was delivered by caesarean section because I had a complete placenta previa - my placenta lay covering my cervix. Now, this is a classic "real" justification for c-section; if I had gone into labor, I almost certainly would have hemorrhaged and died. So I was happy to have the section,
But when it was time to have my second child, I chose to have a vaginal birth. And they warned me up and down about the (very rare) risks, like uterine rupture, but hardly said anything about the risks of having major abdominal surgery! A big reason that I chose to go for the VBAC was that I'd like to have three or four children, maybe even five, and the increase in uterine scar tissue makes each successive c-section more difficult to perform and therefore more dangerous. Whereas each successive VBAC is safer.
Post your comments