At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What are the Different Types of Postherpetic Neuralgia Treatment?
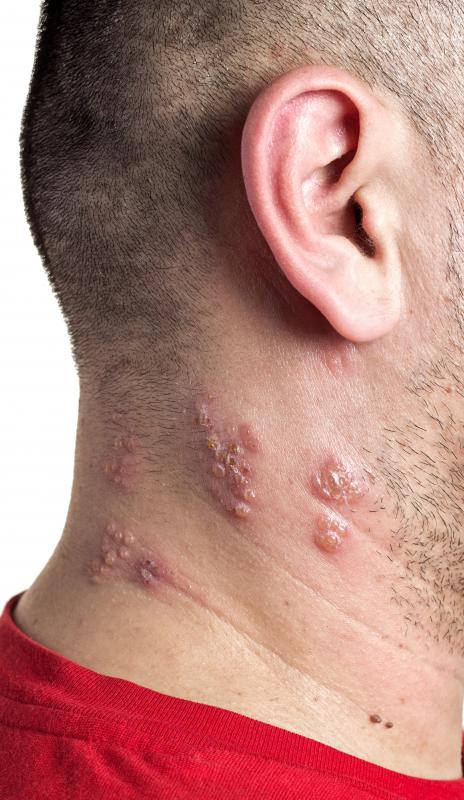
Typically, different types of postherpetic neuralgia treatment includes oral, topical, and injectable medications as well as nerve-stimulation treatments. Postherpetic neuralgia occurs as a complication of the shingles virus. Shingles is a second occurrence of the chickenpox, or varicella virus.
Generally, when an individual gets chickenpox, a portion of the viral infection stays in the body, staying dormant in the nerve cells. Years later, a reactivation of the virus can occur, resulting in herpes zoster, or shingles. Unless a person had chickenpox sometime in his life, he cannot get shingles.

Generally, symptoms of postherpetic neuralgia include excruciating burning, sharp or jabbing pain located deep in the tissue or skin. In addition, sensitivity to temperature changes or touch and itching can occur. Sometimes, headache and numbness will be noticed, as will muscle weakness. Frequently, the physician and patient will need to work together, experimenting with multiple methods of pain relief because of the challenging nature of the condition. Although frustrating, postherpetic neuralgia treatment is usually successful in relieving most of the pain, however, complete resolution is sometimes elusive.

Frequently, antidepressant medication is included in the postherpetic neuralgia treatment plan. Although many patients who experience postherpetic neuralgia are not depressed, antidepressants affect brain chemicals such as norepinephrine and serotonin, which plays a significant role in how the body and brain interprets pain. Usually, when antidepressants are prescribed in postherpetic neuralgia treatment, the doses are smaller than they would be if prescribed in the treatment of depression. In addition, antidepressant medication can provide an added benefit of lifting the mood, as severe pain can contribute to feelings of hopelessness and depression in certain patients.
Sometimes, injected corticosteroid medication is used for postherpetic neuralgia treatment. Typically, the steroid is injected directly into an area near and around the spinal cord to alleviate persistent pain. Treating shingles with injectable steroids is usually not done until all pustular skin manifestations that are associated with the disease have gone away. Injecting medication into the tissue before complete resolution of blisters, and before any open areas have completely closed, puts the patient at risk for developing a secondary infection and tissue damage.
Many times, opioid-based painkillers are prescribed in conjunction with other therapies because of the severity of shingles pain. Although these medications can be addictive, generally the risk low. Prescription painkillers are often effective when combined with topical skin patches that contain medication that relieve pain, such as lidocaine or capsaicin. In addition, painkillers are often used in conjunction with electrical nerve stimulation in postherpetic neuralgia treatment. Frequently, nerve stimulation, which utilizes small electrical impulses delivered to nerve pathways, is thought to stimulate endorphins, a natural painkiller in the body that may alleviate severe pain.
AS FEATURED ON:
AS FEATURED ON:











Discussion Comments
I have had a burning itch / pain in my right arm that mimics postherpetic neuralgia symptoms (from what I've read) for seven and a half years; it is from multiple sclerosis. I can't wear a sleeve on it and sometimes I have scratched through the skin.
Thankfully, I have been blessed with a relative who is a nurse practitioner and did some research. She recommended "LIDODERM" which is a lidocaine patch. It is the best thing for this that I have tried (I tried several oral medications and creams - even Lidocaine cream).
I can function much more normally with this and I would highly recommend it (prescription only) to anyone going through this problem. I hope this helps someone else out there; until there is a better solution at least. Have a blessed day.
Post your comments