At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
Can You See a Herniated Disc on an MRI?
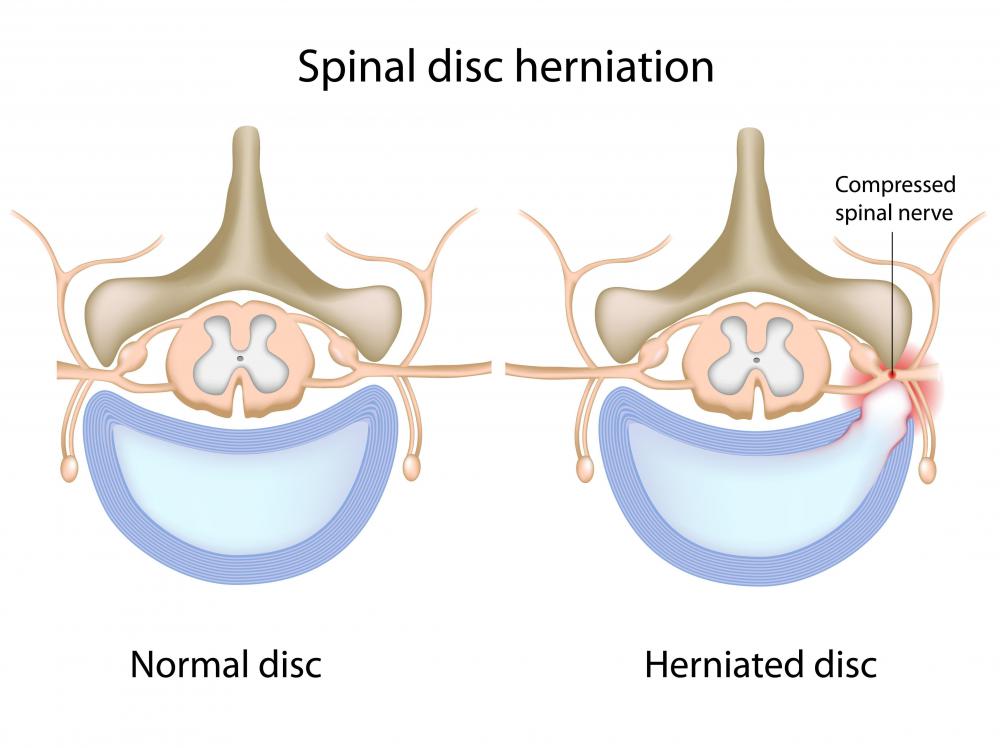
Magnetic resonance imaging (MRI) is the diagnostic tool of choice to determine the presence of a herniated disc. A traditional x-ray shows bony ridges common to spinal injuries and disorders such as cervical spondylosis, but seldom shows soft tissue damage. By comparison, a herniated disc on an MRI shows more details, since such injuries involve damage to soft tissue. Damage to disc material, as well as cord and root compression common to a herniated disc display better and with more detail on an MRI image.
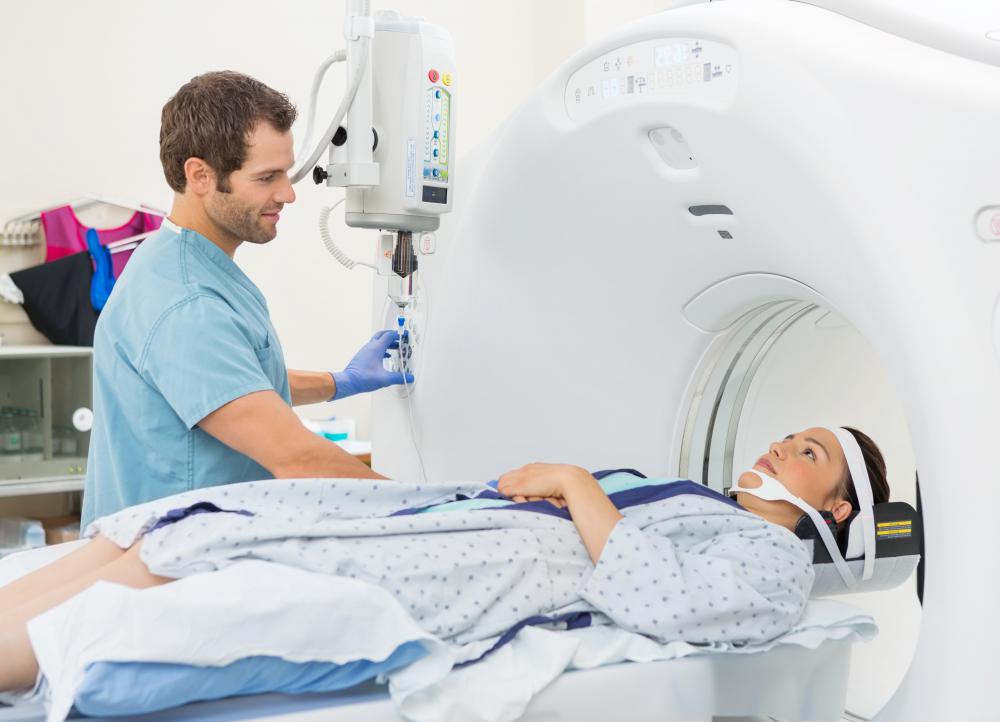
In diagnosing back pain, patients first sit for a series of traditional x-rays to rule out bone-related causes for the pain. These x-rays indicate wear and tear on bony structures of the spine as well as possible injuries or degenerative spinal diseases. The next step is an MRI scan to assess the condition of soft tissue such as discs. For the patient, looking for the cause of the pain such as a herniated disc on an MRI is as painless a having an x-ray. In terms of diagnosing herniated discs, an MRI provides more accurate imagery than CAT scans or a myelogram.

Historically, before the popularization of using MRIs to diagnose soft tissue damage, myelograms and CAT scans were the test of choice to find injuries such as herniated discs. While still in use today, these tests are not as effective due to the lack of detail available in the images created. A myelogram involves injecting a specially formulated dye into the spinal canal. Through fluoroscopy, a special type of x-ray, doctors use the dye as a contrast material to highlight any abnormalities.

Seldom is a myelogram enough to confirm the presence or severity of a herniated disc. A CT scan is normally required immediately following the myelogram, while the dye is still present in the spinal canal. By contrast, a herniated disc is immediately visible on an MRI with no additional testing needed for most patients. Not only is the image of a herniated disc on an MRI more readily visible and detailed, but the patient need not endure any form of injection or invasion of the spinal canal.

By finding a herniated disc on an MRI image, doctors reduce the number of tests a patient must endure to only two. The cost of using just x-rays and MRI scans is less than using x-rays, myelograms, and CT scans. Results are more accurate, immediate, and cost less both in monetary fees, time, and patient discomfort.
AS FEATURED ON:
AS FEATURED ON:














Discussion Comments
@anamur-- You might want to read the wiseGEEK article on "What is a herniated disc?" I didn't understand how herniated discs are diagnosed until I read that one as well.
From what I understand, a herniated disc is when a spinal disc cracks and releases spinal fluid. The fluid applies pressure on nearby nerves and causes pain. An x-ray will show the discs but it won't show the fluid. That's where an MRI comes in.
MRIs are kind of cool. It's not like an x-ray. It's like an active image that shows both hard and soft tissues. Mine was like a short film.
What does magnetic resonance imaging look like?
And why can't we see herniated discs in x-rays? As far as I know, spinal discs do show on x-rays.
A herniated disc in my back was diagnosed with an MRI last year. My doctor didn't even ask for x-rays. He did a physical exam and said that all the signs point to a hernia and ordered an MRI right away.
He was right. I had the MRI and my doctor saw the hernia in the imaging. He even showed it to me on his computer and gave me a CD with it. I keep it in my medical folder at home.
Post your comments