At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What is Vaginal Vault Prolapse?
In a vaginal vault prolapse, the upper section of the vagina is no longer supported and begins to sag into the lower section. This problem happens most commonly in hysterectomy patients. Normally, the uterus sits at the top of the vagina and helps to keep it in position; when the uterus is removed, that support is removed and the vagina can collapse inward. It may fall into the lower portion of the canal, or may even protrude through the vaginal opening.
Though hysterectomy is the most common cause, other issues may contribute to prolapse as well. Weakening or damage of the ligaments and muscles supporting the vagina and other surrounding structures such as the uterus, bladder, and rectum may also allow the vagina to sag; often childbirth is to blame for this. Activities that put stress on that area of the body may also exacerbate the problem. Often vaginal vault prolapse occurs along with prolapse of other nearby organs.

Women with vaginal vault prolapse may have a variety of symptoms. They may experience a feeling of achiness, discomfort, or heaviness in the pelvic region, aching in their lower back, and pain during intercourse. The bulging of the vagina's upper part into the lower section may make movements such as standing or walking difficult. Sometimes vaginal bleeding may occur, and the opening may gape widely. Pressure on or prolapse of the nearby bladder may lead to incontinence, and some women have recurring urinary tract infections as well.

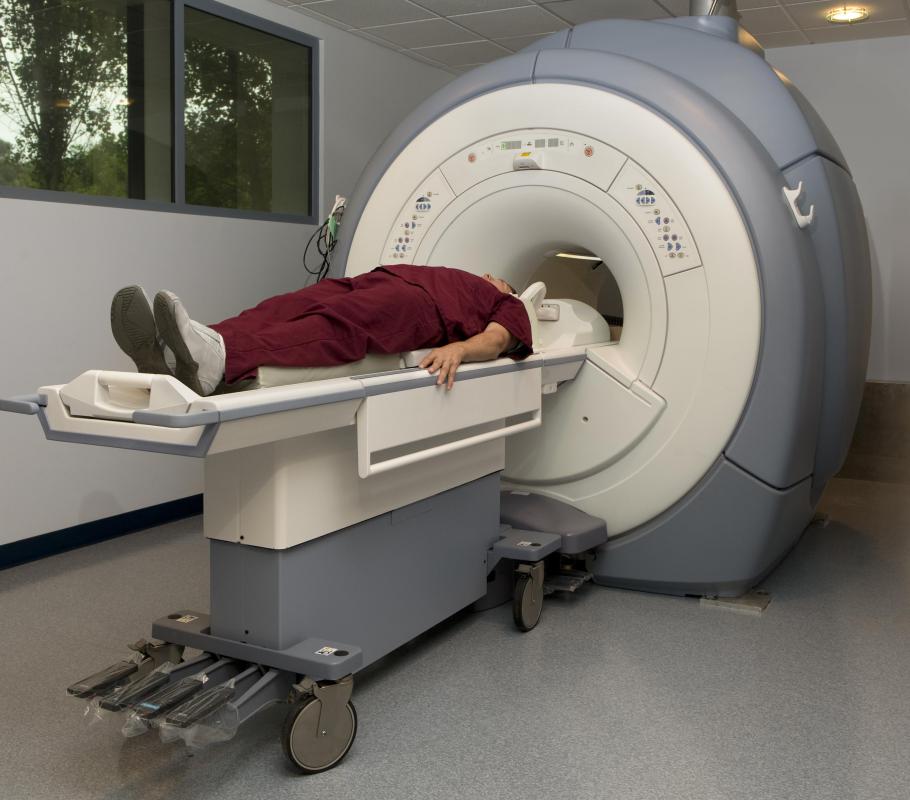
To diagnose a prolapse, a doctor will typically start with a review of the woman's medical history. This will usually be followed by a physical exam of the vagina. In some cases, an MRI or ultrasound may be used to give a better view of the vagina and surrounding tissues, particularly if prolapse of any surrounding structures is also involved.
Surgery is typically required to repair a vaginal vault prolapse. This type of surgery is sometimes called colpopexy, vaginopexy, or vaginofixation. There are two main types; the first, vaginal sacrospinous colpopexy, involves entering the body through the vagina and attaching it to the sacrospinous ligament. The second type, abdominal sacral colpopexy, is when the surgeon goes in through an incision in the abdomen and sutures a mesh in place to hold the vagina in the correct position.
AS FEATURED ON:
AS FEATURED ON:
















Discuss this Article
Post your comments