At WiseGEEK, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What Is Thromboxane A2?
Thromboxane A2 is a member of the group of lipids known as eicosanoids, which act as signaling molecules in the human body. The thromboxane family of eicosanoids also includes thromboxane B2. Activated platelets use the enzyme thromboxane-A synthase to convert prostaglandin H2 to thromboxane A2. The lipid then helps clot formation by stimulating the activation of more platelets, increasing their aggregation, and acting as a vasoconstrictor to narrow blood vessels. Many anticoagulant drugs act against either the formation of or the function of this molecule.
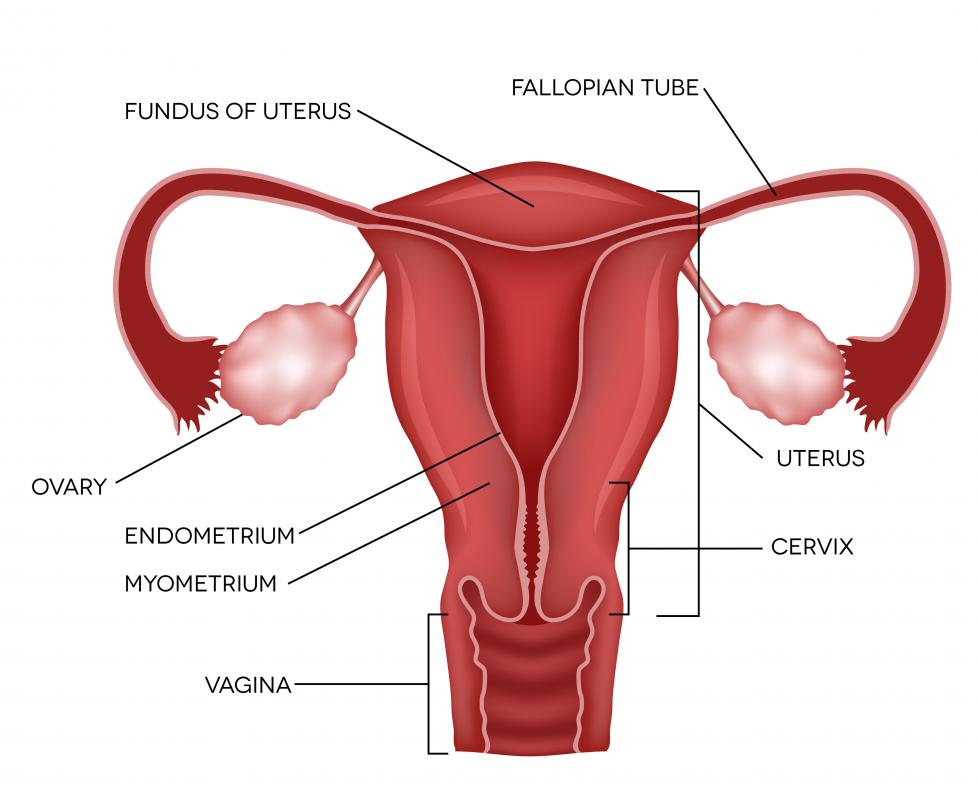
The four families of eicosanoid lipids are the prostacyclins, the prostaglandins, the leukotrienes, and the thromboxanes. Eicosanoids serve as signaling molecules for body processes such as smooth muscle contraction, clot formation, inflammation, and uterine contraction. Thromboxane A2 is a key component in clot formation, and thromboxane B2 is its inactive metabolite. Since the active form is very unstable, scientists often test thromboxane B2 levels as an indication of thromboxane A2 production during research studies.

Arachidonic acid is a lipid found in foods such as red meat and eggs. In the body, the proteins cyclooxygenase-1 and cyclooxygenase-2 (COX-1 and COX-2) catalyze reactions in which arachidonic acid is converted to prostaglandins. Prostaglandin H2 is the precursor of thromboxane A2.
During the process of clot formation, thrombin activates platelets at the site of the injury. The enzyme thromboxane-A synthase, which is present in the activated platelets, converts prostaglandin H2 to thromboxane A2. This molecule then activates more platelets, producing a positive feedback loop that forms a blood clot. The lipid also causes the injured blood vessel to constrict, further inhibiting bleeding.

Since this molecule is so important for clot formation, it is the target of many anticoagulant drugs. Aspirin, for example, irreversibly inactivates the COX enzymes and prevents thromboxane production by preventing the production of prostaglandin H2. Other nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen also reversibly inactivate the COX enzymes. Some anticoagulants inhibit thromboxane-A synthase, and others are thromboxane A2 receptor antagonists.

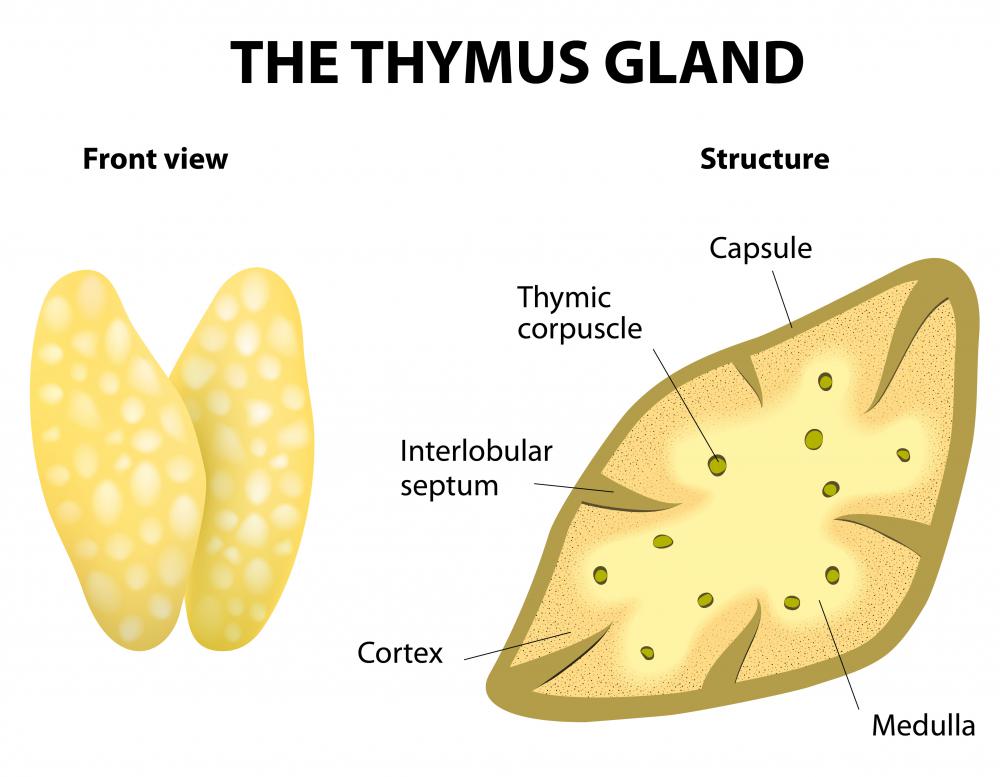
Clot formation was the most understood of thromboxane A2's functions as of early 2011, but the activities of the eicosanoids and their interactions with other molecules in the body are very complex. Some studies indicate that it might interact with thrombin to stimulate the proliferation of new smooth muscle cells within damaged artery walls, thus taking an active role in blood vessel repair. Other studies have found that receptors for this molecule in the thymus gland might play a role in apoptosis (programmed cell death) of certain cells in the thymus. Thymocyte apoptosis is associated with immune problems and a low survival rate for patients who have sepsis, so further study in this area could prove valuable for the care of these patients.

Receptors for thromboxane A2 are abundant in the lungs and spleen as well as the thymus, and the molecule's functions in those organs are still poorly understood. Further intensive study the receptor functions within different organs and of the eicosanoid's interaction with other molecules is likely to illuminate the complex roles that this important molecule plays within the human body. This knowledge could be invaluable in the development of new medications.
AS FEATURED ON:
AS FEATURED ON:















Discuss this Article
Post your comments