At WiseGEEK, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What is Pericardiocentesis?
A surgical procedure used to remove fluid from the pericardial sac of the heart is known as pericardiocentesis. The procedure is generally conducted to determine the cause of recurrent pericarditis, a condition which contributes to the inflammation of the pericardium, or pericardial sac. As with any medical procedure, there are risks associated with pericardiocentesis and these should be discussed with a qualified health care provider prior to surgery.
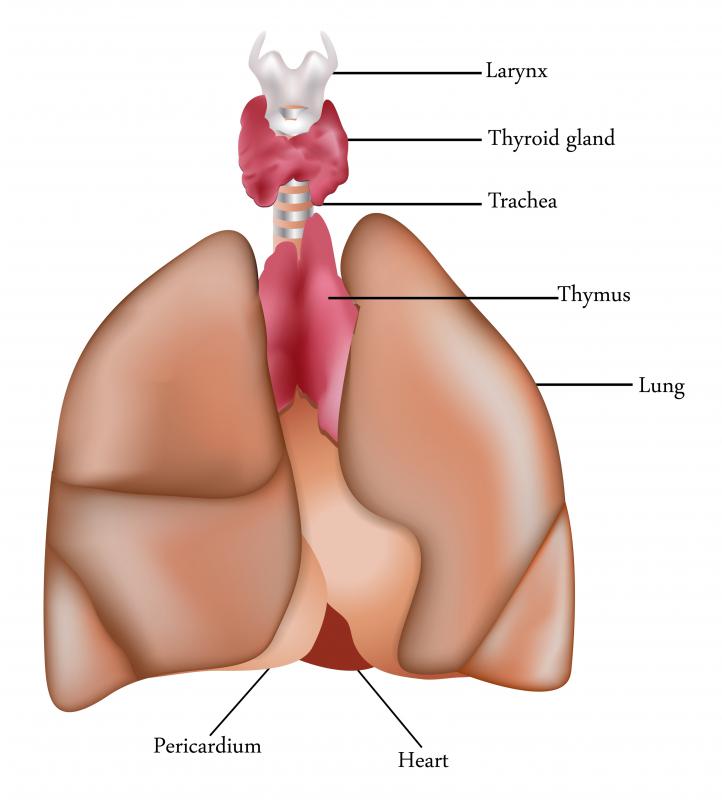
Individuals who become ill from a viral or bacterial infection may develop complications which include the inflammation of the pericardium, or the sac that surrounds the heart. Known as pericarditis, this disorder is sometimes associated with conditions such as autoimmune disorders, rheumatic fever, and HIV/AIDS. Those who have experienced a recent heart attack, undergone radiation therapy, or have sustained trauma to the upper torso, including the chest and heart, may develop pericarditis. In most cases, the reason for the development of this condition may be idiopathic, meaning there is no clear cause.

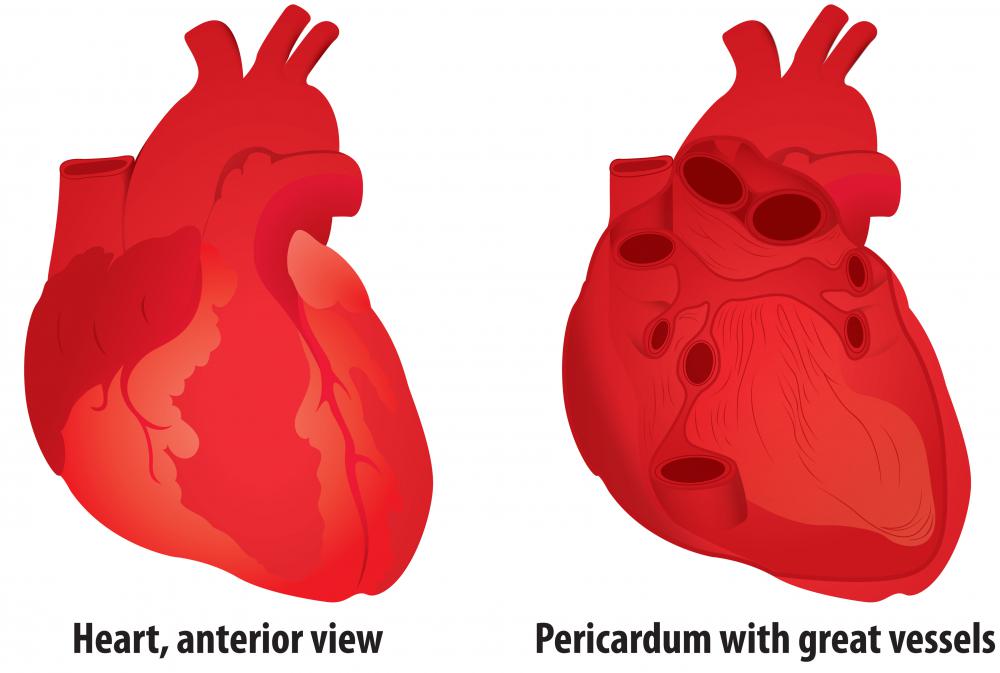
Fluid naturally surrounds the heart muscle and works to lubricate and cushion it, promoting proper functioning. In situations when too much fluid builds up in the sac, such as with an infection, it can cause pressure to build up around the heart. The collection of too much fluid around the heart may cause the individual to experience chest pain or discomfort. In some instances, the individual may be asymptomatic, meaning he or she may not exhibit any symptoms at all.

A pericardiocentesis procedure involves the insertion of a hollow needle into the pericardial sac to remove the built-up fluid. Commonly conducted in the intensive care unit (ICU), the individual will be given an IV as a precautionary measure in the event the administration of medications may be necessary. A local anesthetic, or numbing medication, is administered at the designated insertion site.

The area directly below the breastbone is washed with a sterilizing agent prior to the insertion of the surgical needle. Echocardiography, a form of guided imaging that employs sound waves to generate a picture of the heart, is utilized to properly guide the needle to the target area and monitor the flow of fluid during the removal process. Once the needle reaches the target area, it may be removed and replaced with a thin tube commonly known as a catheter. In some cases, the hollow needle may remain in place and used to draw off the fluid from the pericardium. The fluid collection process may take several hours to complete or, in some cases, several days.

Normal results associated with this procedure generate a small quantity, considered to be 0.3 – 1.7 fluid ounces (about 10-50 ml), of translucent, pale, yellow-colored liquid that contains no blood, infection, or cellular abnormalities. A large amount of fluid, more than 1.7 fluid ounces (about 50 ml), drained from the area is considered to be abnormal and indicative of a more serious condition. Submitted for laboratory analysis, the fluid may indicate the presence of various conditions, including congestive heart failure, cancer, or certain systemic diseases, such as lupus.

A pericardiocentesis procedure is considered to be relatively painless. The individual may feel a bit of discomfort during the initial administration of the local anesthetic. He or she may feel a bit of pressure during the insertion of the needle or experience mild chest discomfort, in which case pain medication may be given intravenously. Risks associated with a pericardiocentesis include infection, heart attack, and irregular heartbeat, known as a heart arrhythmia. In rare cases, the coronary artery, lung, or heart muscle may be punctured during the needle insertion process.
AS FEATURED ON:
AS FEATURED ON:















Discuss this Article
Post your comments