At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What is a Rectal Prolapse Repair?
A rectal prolapse repair is a surgical procedure performed to treat a rectal prolapse, in which the end of the intestines protrudes out the anus. Surgery is not usually the first line of treatment for prolapses of the rectum, except in special circumstances, and is generally presented as an option after other treatment methods are ineffective. The procedure is performed in a hospital or well equipped clinic and, as with other surgical procedures, there are some accompanying risks that should be considered before surgery.
A rectal prolapse is an extremely uncomfortable condition, and it can expose people to risks of infection and other complications. The first treatment usually involves manually pushing the prolapsed material back into place and then determining why the patient developed a prolapse. Treatment of the underlying cause can include providing patients with a high fiber diet to address constipation so that patients don't strain when passing stool.

If rectal prolapse becomes recurrent or it is evident that the tissue is damaged, a rectal prolapse repair must be considered. Surgeons can enter through the abdomen or the area around the anus, depending on the patient and the case. Historically, abdominal surgery for rectal prolapse repair was very invasive. Today, surgeons usually use laparoscopy, making a series of small incisions to introduce tools and a camera to conduct a minimally invasive surgery.

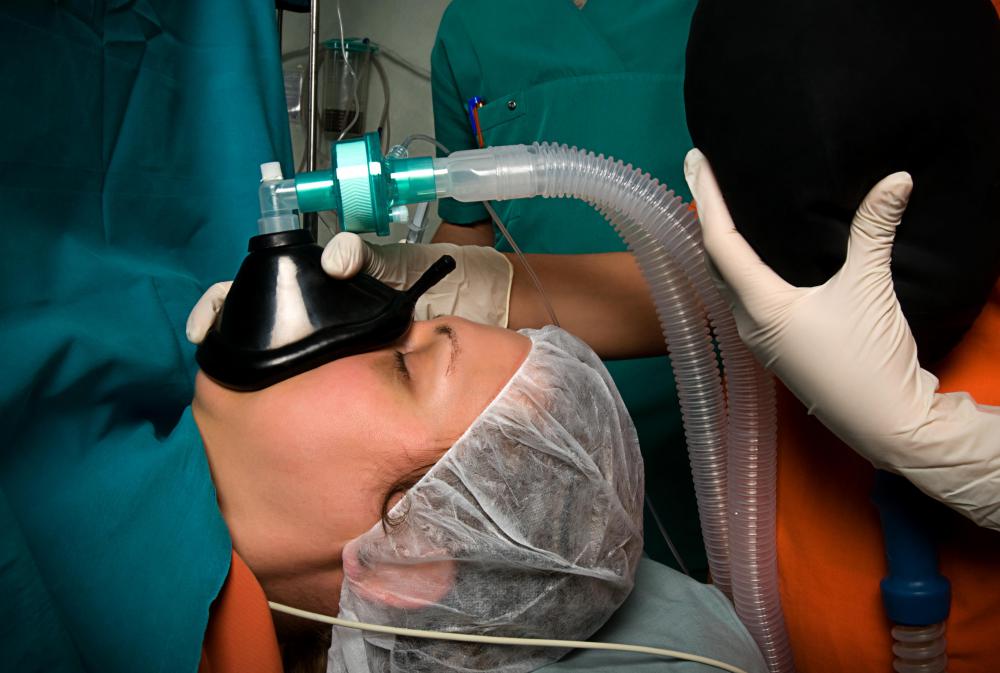
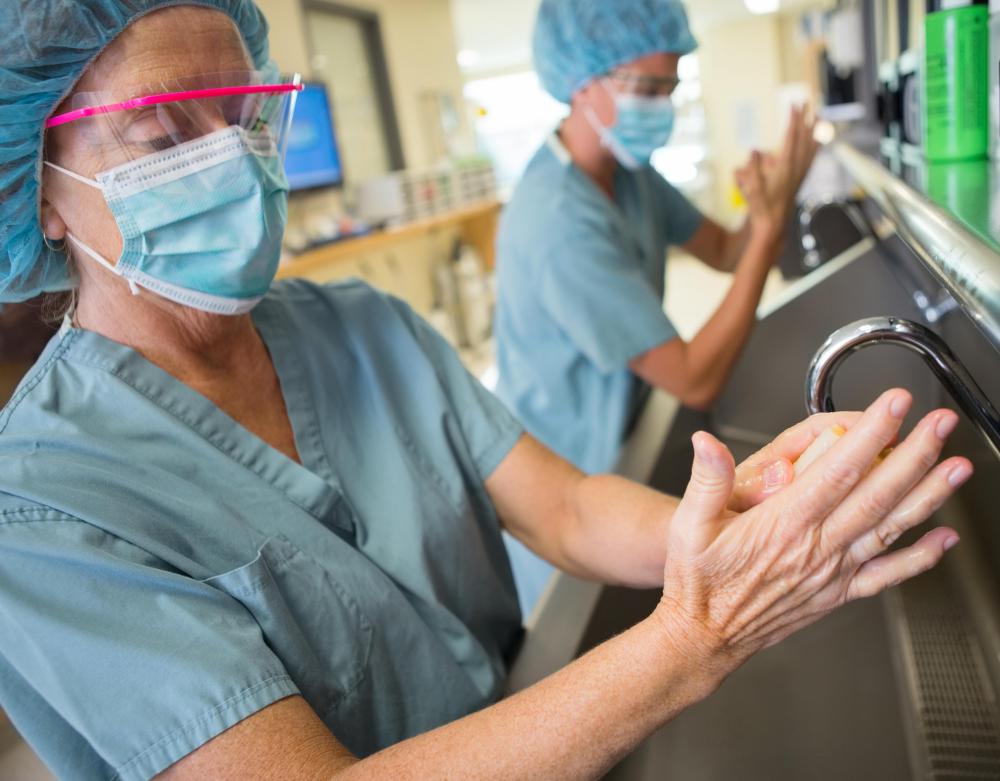
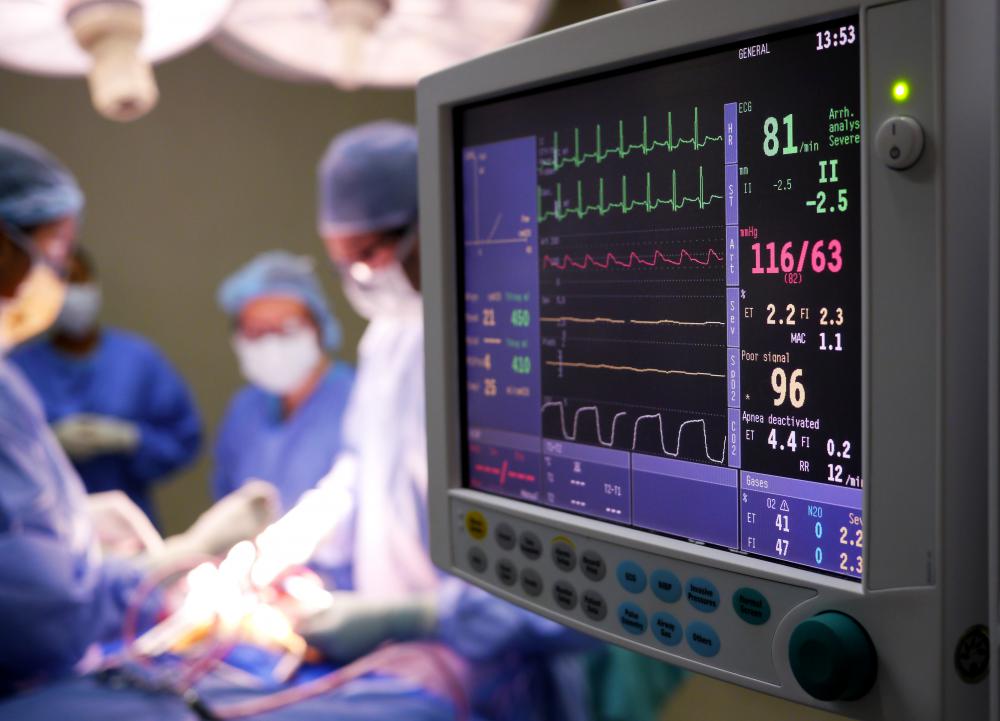
The patient is under general anesthesia while the the surgeon performs the procedure. Once the patient wakes up and is taken into recovery, she or he will be monitored and aftercare directions will be given. Patients may need to eat a special diet while the surgical site heals and they must use special care when washing to keep the site clean.
The main risk of a rectal prolapse repair is infection, usually the result of conditions after the surgery that make the patient susceptible to infection. Anesthesia can also be dangerous for some patients and careful screening is conducted before surgery to confirm that a patient is a good candidate for anesthesia. Other risks can include tearing of the rectum, a recurrence of the prolapse, and incontinence in the wake of the procedure. Working with an experienced surgeon can dramatically reduce risks for patients.

When this surgery is recommended, patients may want to ask why it is being recommended and if there are any alternative treatment options. Meeting with several surgeons and discussing the different approaches to rectal prolapse surgery and aftercare can provide patients with more information they can use to make an informed decision about a rectal prolapse repair.
AS FEATURED ON:
AS FEATURED ON:














Discussion Comments
A proctologist has recommended low anterior colon resection (rectopexy) for my (severe) rectal prolapse. I have almost no discomfort from this situation; don't strain when having a BM (which I have from 4-5 times a week) - and I'm always able to push it back in afterward.
From what I've read about the surgery, there are a number of risks and the prolapse could still return. I feel fine now. What should I do?
Post your comments