At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What is a Pathological Fracture?
A pathological fracture is a break in a bone that occurs as the result of an underlying disease as opposed to direct physical trauma or impact. In fact, most pathological fractures occur spontaneously during normal activity, or after a mild injury that wouldn’t ordinarily lead to a broken bone in most people. A significant loss in bone density due to the development of osteoporosis is most frequently to blame. However, there are many other conditions that can lead to a pathological fracture, including metabolic disorders, genetic bone deformities, infection, benign tumors and cysts, and cancers that have metastasized to the bone.
Prevention is important for a variety of reasons, not the least of which is the avoidance of pain and decreased mobility. However, for those who may be at increased risk, taking a proactive approach to reduce the likelihood of a pathological fracture occurring also translates to fewer surgical interventions and lengthy hospital stays. Regular screening for patients who present one of the previously mentioned risk factors is recommended, particularly if there is reason to suspect skeletal lesions.

Often, the only symptom to occur is localized pain that does not respond to anti-inflammatory drugs or pain blockers. In addition, it should be noted that pain from skeletal lesions might initially be attributed to other conditions and overlooked. For instance, metastases impacting the spinal cord or pelvis region are often mistakenly attributed to sciatica.

Diagnostic measures used to detect pathological fractures typically begin with blood tests. Elevated levels of c-reactive protein and erythrocyte sedimentation, for example, indicate the presence of a chronic inflammatory condition. Urine analysis may also be performed to assess levels of n-telopeptices, which serves as a gauge to the rate of collagen deterioration in bone.

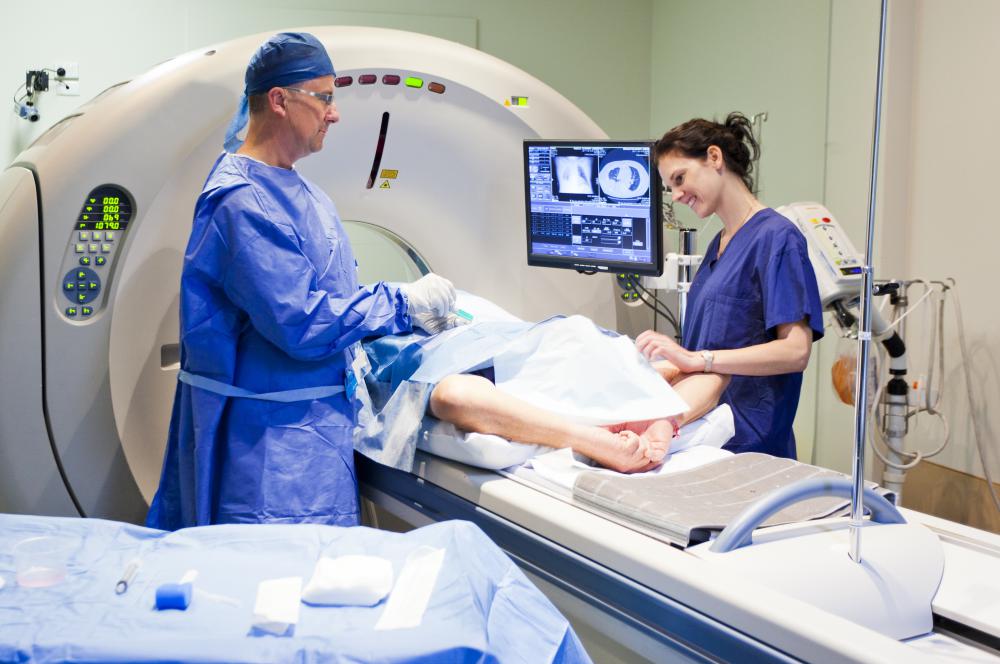
Magnetic resonance imaging (MRI) and computed tomography (CT) scans usually follow, which reveal the rate of marrow replacement and the details of bone structure, respectively. When tumor formation is suspected from these tests, a radionuclide scan of the entire body may be performed to pinpoint specific locations where a pathological fracture is most likely to be found or to occur at some later point.

Treatment varies with each individual. In some cases, chemotherapy or radiation may be necessary to reduce tumors. Patients who experience a pathological fracture due to bone metastases associated with breast cancer are often treated with bisphosphonates. Surgery may also be indicated. For instance, some patients may benefit from prophylactic fixation of the fracture site with bone cement and rods, while others may receive an artificial prosthesis to replace defective bone.
AS FEATURED ON:
AS FEATURED ON:
















Discussion Comments
@fify, @turkay1-- Disease is a special circumstance and I'm sure those treatments do help. But many times pathological fractures happen simply from old age, poor nutrition and lack of safety. I work in a nursing home and this is a problem that many of our residents deal with or have dealt with before arriving.
I think the best prevention method is making sure that we consume a healthy nutritious diet and get plenty of calcium and vitamin D which is necessary for our bones. For elders, we need to get safety rails for their home, especially for bathrooms and stairs. Even a minor fall can lead to a fracture in an elder person like the article said.
The residents at our nursing home are mostly over the age of seventy. This is when the risk of fractures are the highest. We have to pay close attention to all these factors for this reason.
@fify-- I don't know if this was available during your grandmother's tumor treatment. But recently, doctors use radiotherapy when there is bone metastases to help prevent pathologic fractures that may develop in the future.
It's not a 100% guaranteed treatment but it has shown to assist with pain in bones after tumor treatments. And it is almost always applied in these circumstances now.
They release a radioactive drug into the bloodstream during this therapy and it helps prevent the tumor from spreading and further damaging the bone.
If possible, preventing an impending pathological fracture is the best thing to do.
I know how painful and complicated pathological fractures can be from my grandmother who suffered from one two years ago. She had a tumor in her hip which was treated about four years ago. The tumor is gone but it left her hip bone very weak and she developed a pathological fracture soon after.
The doctors had to put in a nail to keep the bone together which didn't work. The nail broke and she got an infection in that area. The doctors removed the nail and are treating her with antibiotics. But my grandmother can't walk and has chronic pain in the area. Her doctors haven't decided what the next step should be in her treatment.
It's really frustrating for me and my parents because we want her to be well. Pathological fractures are no picnic. I wish we had been able to prevent it when she was diagnosed with the tumor although I'm not sure how we could have done that.
Post your comments