At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What Is a Liver Abscess?
An abscess is a pus-filled growth or sack that forms on an organ or tissue in the body, and a specifically liver abscess is one that occurs on or within the liver. In general there are three types. By far the most common is pyogenic, which basically means “pus producing”; these abscesses are usually caused by major bacterial infections or problems with other nearby organs, particularly the appendix. Abscesses can also be amoebic or fungal, and these distinctions are normally drawn based on what caused them — and, relatedly, how they should be treated. In terms of appearance and basic characteristics, though, all are quite similar. They are all caused by bacteria, parasites, or fungal spores that trigger an immune response that gets out of hand and leads to a buildup of puss and other fluid. Physicians usually start out treating abscesses on the liver with antibiotics, but in advanced cases they may need to be drained or repaired surgically.
Primary Abscess Types

Most experts estimate that upwards of 80% of detected liver abscesses are polymicrobial pyogenic abscesses. These are caused by major strains of well-known bacteria and tend to produce their own pus as well as absorbing the pus produced as a natural byproduct of its growth and development. Pus is usually thought of as trapped tissues and dying cells that are cut off from oxygen in a cyst, growth, or site of infection. The bacteria that cause this sort of abscess can come from various sources. An abdominal infection, such as an infection of the appendix or bowel, is one example; a perforated bowel, where leakage from the colon into the abdominal cavity occurs through a small tear, is another.

Less common are amoebic and fungal abscesses. Most amoebic cases are caused directly by a specific parasite known as Entamoeba histolytica. The parasite lives in the bowel but can spread to other organs depending on how it entered the body. Fungal abscesses, as their name might suggest, are typically tied to fungal spores of the genus Candida, which is a yeast. In all cases, the problematic substance, be it a bacteria, a parasite, or a fungus, attaches itself to the liver wall and causes a pocket or pouch to form as the immune system tries to isolate and destroy it. It’s usually very hard to identify what caused the abscess until it’s been biopsied, though a blood test will often give some strong clues.
Understanding the Liver Generally

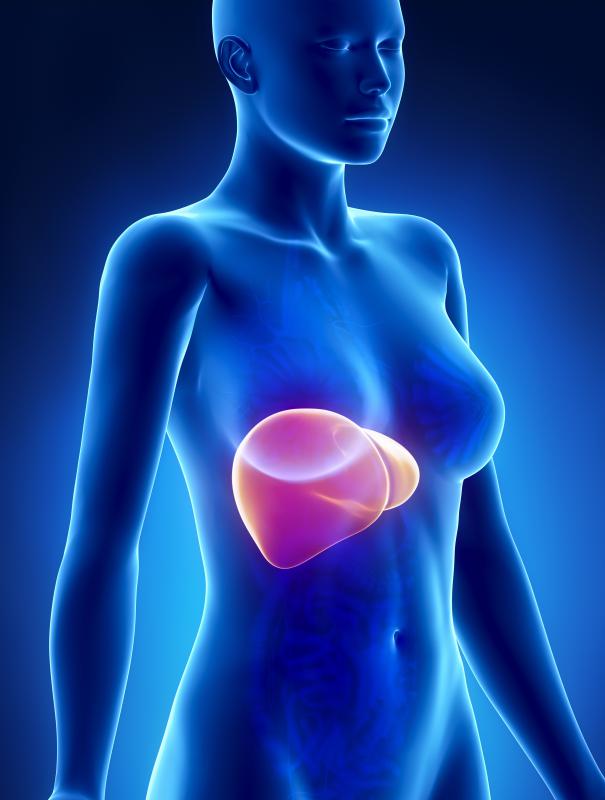
The liver is a complicated, hard working organ located in the upper right quadrant of the abdominal cavity in humans. Although it performs over 500 functions, the major ones are to filter the blood and remove chemicals and toxins. It regulates the metabolism of the body, and assists in the breakdown of fats in foods for proper function of the digestive system. It is the only organ in the human body capable of regeneration, unless liver disease becomes so severe it is unable to recover. The liver is composed of two lobes that work independently of the other, and if one lobe is damaged, the other lobe can keep functioning on its own.
Abscesses don’t always present symptoms right away, and as such they can be hard to detect at first. A lot depends on where on the organ the pouch forms, and how big it is.
Main Symptoms

The most common symptoms of a liver abscess include chalk-colored stools, fever and chills, abdominal pain, and a yellow cast to the skin known as jaundice. If any of these symptoms are experienced, medical attention should be sought immediately. Treatment can consist of a long-term regimen of antibiotics, usually lasting four to six weeks, and sometimes this is enough to resolve the condition. Other treatment options include surgery or the insertion of a needle to drain the abscess. Even with proper treatment, it’s estimated that only 10 to 30% of people with a liver abscess experience life threatening complications, such as sepsis, a potentially lethal blood infection.
Diagnosis

Common tests a doctor might perform when an abscess on the liver is suspected include an abdominal computed tomography (CT) scan, similar to an X-ray, and an abdominal ultrasound. Blood tests, such as a white blood cell count to assess the level of infection, a blood culture to identify the bacteria causing the infection, and blood tests indicating liver function, will also usually be performed. A biopsy of the liver may also be indicated in some instances. Although prompt treatment of any abdominal infection can reduce the risks of developing a liver abscess, the condition isn’t always preventable.
AS FEATURED ON:
AS FEATURED ON:















Discuss this Article
Post your comments