At WiseGEEK, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What is a Citrate Anticoagulant?
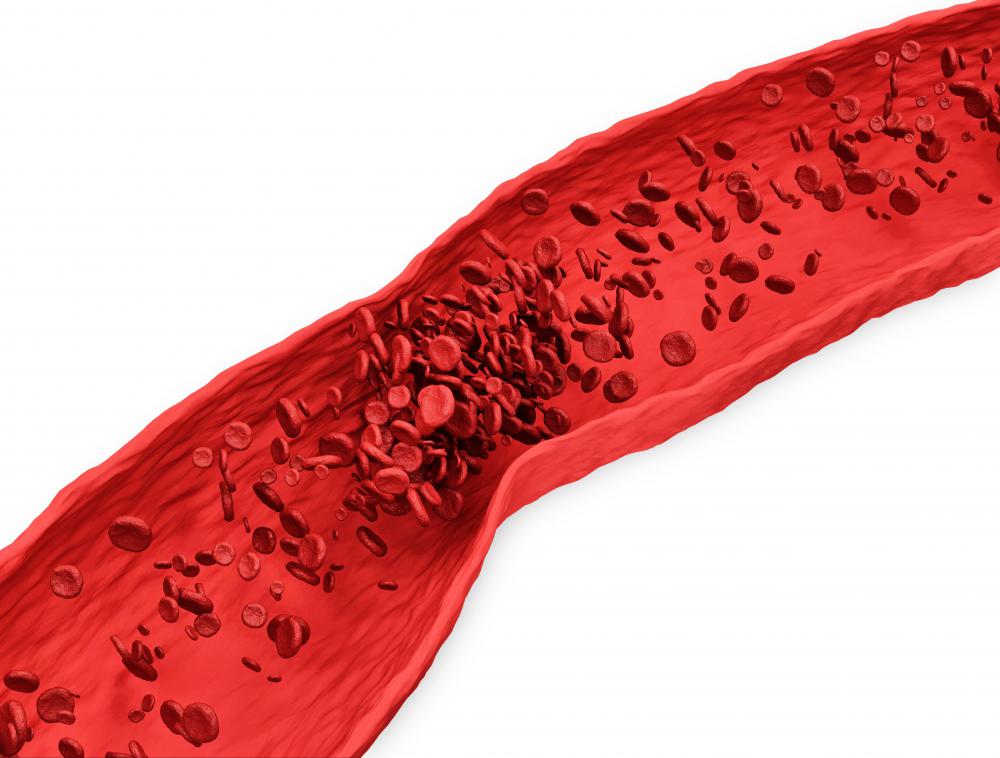
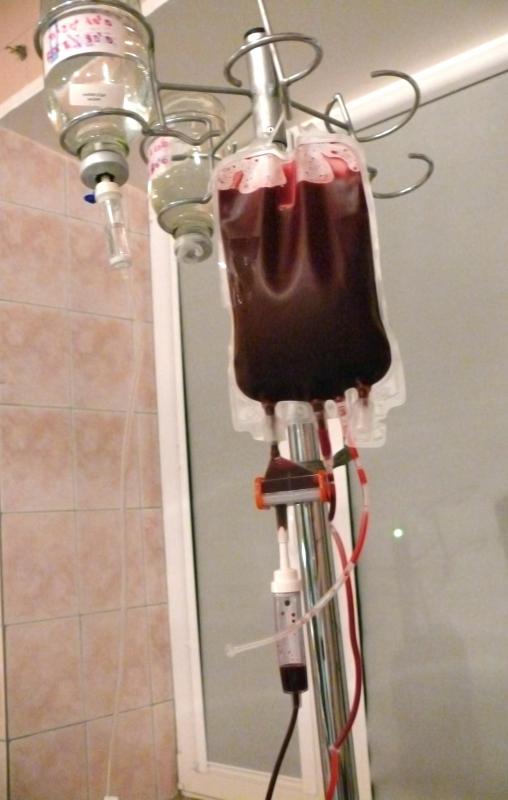
A citrate anticoagulant is used to thin the blood and prevent clotting. Unlike many anticoagulants, citrate anticoagulants cannot be administered directly to a patient, though they may enter a patient's body when mixed with blood given as a transfusion. The primary use for this type of anticoagulant is to prevent clots in blood that is being held in test tubes or transfusion bags. By binding to calcium, which is a mineral required for the thrombin cascade, citrate anticoagulants stop blood clots from forming. The thrombin cascade is a series of chemical interactions that cause a blood clot to form.
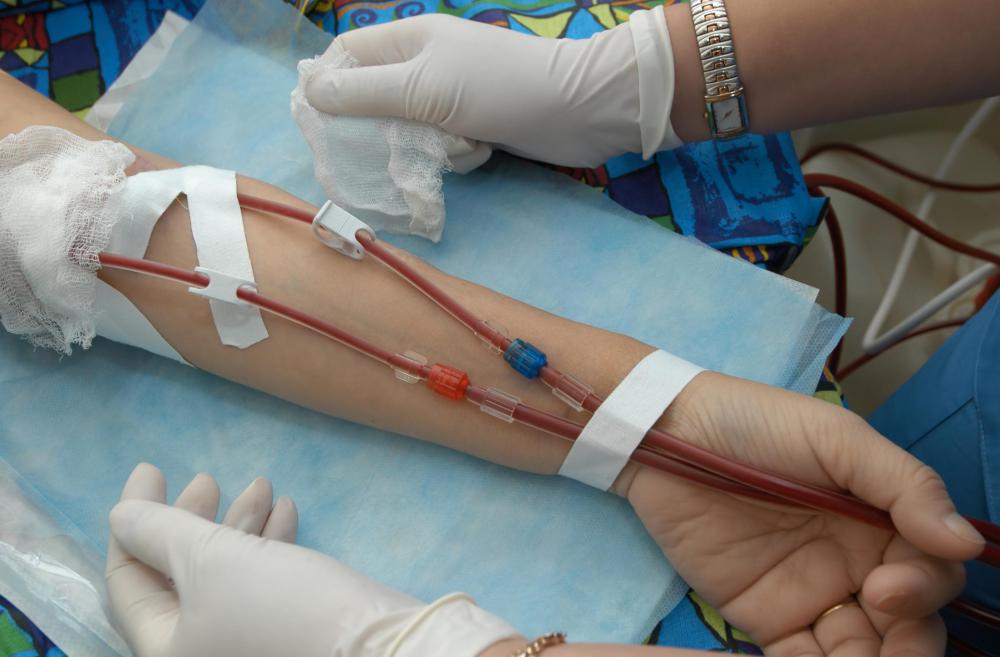
Administering citrate anticoagulants directly to a patient can pose a serious health risk, so they are only used to prevent blood clots that are outside the body. A filter installed in blood transfusion bags removes some of the calcium citrate molecules from the blood before it reaches the patient. Though not all of the anticoagulant is removed, the amount remaining is usually not enough to significantly thin the patient's blood. Patients suffering from some types of organ failure, however, such as liver failure, may be at risk of severe bleeding if given a transfusion of blood that has been treated with a citrate anticoagulant.

Two types of citrate anticoagulant are available. One is called anticoagulant acid citrate dextrose. This compound contains citric acid, trisodium citrate, and dextrose. Trisodium citrate acts as an anticoagulant, while the citric acid is used to ensure that the blood is at the proper pH. The dextrose in this mixture is useful as a source of energy and also helps keep red blood cells from breaking down. Variations of this compound may include phosphate, to improve the shelf-life of blood, or adenine, to help keep adenosine triphosphate (ATP) levels high.

The other type of citrate anticoagulant is called anticoagulant sodium citrate. This compound uses sodium citrate for its capacity to interfere with thrombosis. It is used when collecting plasma, the liquid in which blood cells are suspended. Sodium citrate helps to keep the blood thin while the plasma is extracted, before the cells and other solid components are returned to the donor.
AS FEATURED ON:
AS FEATURED ON:













Discussion Comments
What I fail to understand in this is, though both citrate anticoagulation procedures are well accepted, who decides which procedure to go with? Is it possible to go with 4 percent TSC as an anticoagulant, and the only reason for the addition of dextrose is to compensate for the glucose loss, then dextrose if required can be given by a different line?
Moreover, if dextrose is already present in the dilution fluid, then why add additional dextrose? The cost of therapy will only increase. Why can't we just use 4 percent TSC in WFI straight away?
Post your comments