At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What Causes Abdominal Scar Tissue?
Abdominal scar tissue occurs when fibrous tissue, a type of connective tissue, becomes scarred between the abdominal cavity’s structures. Depending on the situation, this scar tissue is often referred to as adhesions, fibrous scar tissue, or fibrosis. Some of the most common causes of scar tissue in the abdomen include surgery, inflammation associated with certain medical conditions, and even treatment for other health problems. Unfortunately, side effects ranging from cramps to intestinal blockage can accompany fibrous scar tissue. Surgery isn’t always an option to remove the tissue, but patients can find relief with certain types of physical therapy.
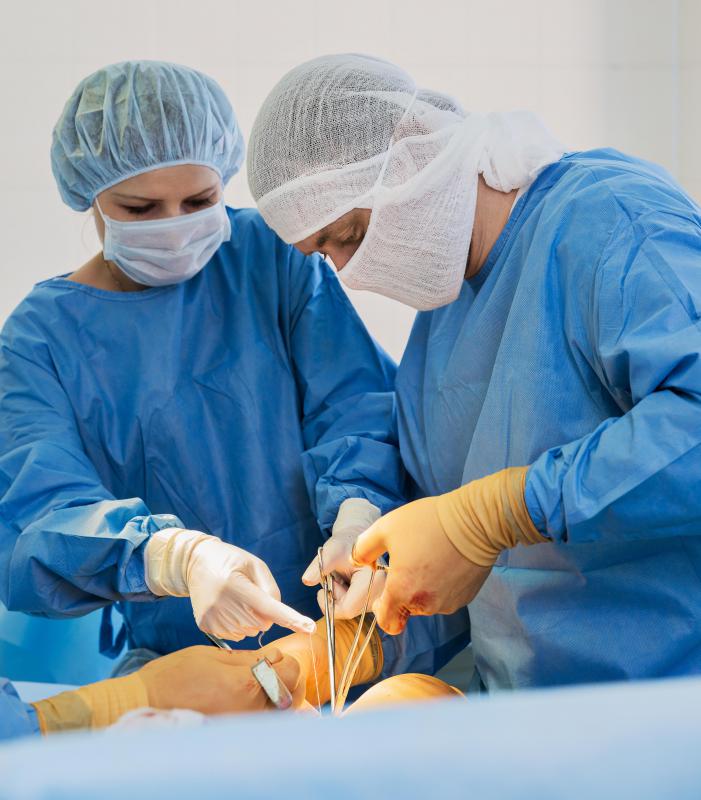
Surgeries can cause abdominal scar tissue beyond the typical types of scar tissue doctors and patients normally expect from incision sites. When scar tissue forms as a result of surgery, it means the patient experiences fibrous tissue scarring that extends beyond the normal incision site scar. Not all reasons for the formation of fibrous scar tissue in response to surgery are understood, but one of the most common is when the tissues become dry during the surgery. These tissues can become dry by accident due to the arid conditions during surgery, or on purpose when the surgeons use gauze and other materials to improve their view. Open abdominal surgery, called laparotomy, results in these kinds of fibrous tissue scars more often than laparoscopy, which involves only a tiny incision in the abdomen’s skin.

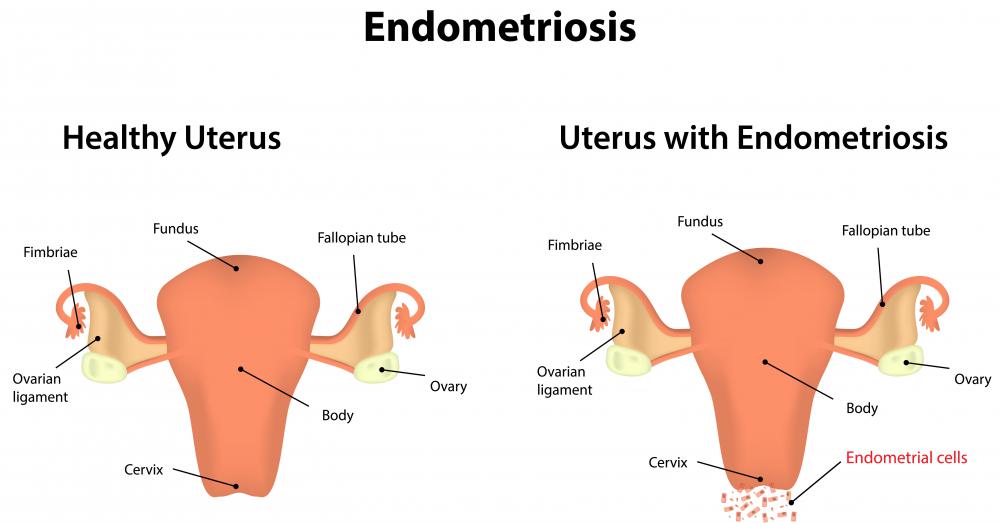
Medical conditions that involve inflammation and infection can eventually lead to abdominal scar tissue. For example, when a person’s appendix becomes infected and inflamed and he develops appendicitis, the surgery to remove the appendix can cause fibrous scar tissue if his intestines stick to his abdominal wall. Taking surgery out of the equation, endometriosis can cause similar adhesions. When the uterus becomes inflamed, scar tissue can form between the pelvic and abdominal cavities. The same is true for diverticulitus, which can lead the inflamed intestine to cause adhesions that stick to the abdominal wall.

Other kinds of situations that can cause inflammation and, consequently, abdominal scar tissue include the treatment of unrelated medical conditions. For example, radiation to treat cancer is designed to stop cancerous cells from growing, but it can also cause inflammation of healthy tissues, such as intestinal tissues. When this happens, abdominal adhesions can form.

Abdominal scar tissue can cause painful cramping and dangerous intestinal blockage. Surgery is an option for removing scar tissue, but since it rarely works, not all doctors suggest it. Certain kinds of physical therapy exercises can help patients alleviate pain and manage the scar tissue. Most of these exercises focus on stretching. For example, abdominal twists, pelvic tilts, and yoga poses like the cobra pose can lessen the pain and even prevent additional scar tissue from forming.
AS FEATURED ON:
AS FEATURED ON:














Discussion Comments
Scarring can happen from gluten (or lectin) sensitivity, taking maximum dosage of ibuprofen or other NSAIDs over a couple of months, or alcoholism. There may be other causes, but those three seem prevalent.
I am 59 years old. I had a diverticulitis attack a few months ago, and now I have cramping down below. They did a colonoscopy on me and said I had a lot of scar tissue. My uterus is fine. I am bloating up, but have no pain. I'm waiting on the CT scan to come back to find out if there is any blockage. I am not sure what to do.
I recently had a colonoscopy and an upper GI. The doctor who did this procedure said he had to change the scope three times because of abdominal scarring and said I must have had surgery at one time on my abdomen. I've never had any of these surgeries, but two years ago I had a colonoscopy and there was no mention of scarring. I had these tests done because I have diverticula and got diverticulosis and was put on antibiotics and something else.
I am 67 and have had two children. My question is how did I get scarring and what now?
Post your comments